On the Other Side of the Stethoscope: When Doctors Become Patients

Viewing life from another person's perspective often allows us to see and think about things differently, and may affect how we interact with those around us. For a physician, a change in perspective can be especially powerful if it results from experiencing life as a patient. Illness has the ability to profoundly change a physician or a physician-in-training, and the process of transitioning from healthcare provider to patient can be quite eye-opening.
Most physicians do their very best to show compassion, provide support and empathy – but this often is insufficient. Sometimes doctors must look through the eyes of those for whom they care in order to better serve their needs. By being "on the other side of stethoscope" and "wearing a gown," providers can learn to better empathize with patients, and, ultimately more effectively ease the pain of living with disease.
The following are invaluable lessons realized by medical students, residents, fellows and physicians at the Medical College of Wisconsin. Through their experiences as patients, they have identified with their patients and developed a keener understanding of the daily struggles their patients face. And they believe they have become – or are in the processing of becoming – better doctors as a result.
The life-changing stories below have influenced how MCW physicians provide care. We are grateful for their willingness to share their experiences and their lessons learned.
Julie Biller, MD

"Two things in particular happened to me that impact the way I practice medicine: my miscarriage and my carotid artery dissection," shares Julie Biller, MD, MCW professor of medicine (pulmonary).
"I had a miscarriage during my first pregnancy. I began bleeding and called my obstetrician. He was so great. He was so clear in his description of what the potential possibilities were, which really helped reduce my anxiety. He was so great at his communications that it had a lasting impact. People really want to hear, in a clear fashion, what's happening to them – even if there is some uncertainty."
Dr. Biller's second meaningful incident – which she refers to as her "bad haircut story" – occurred 20 years ago. "I had gone to get my hair cut, which for women means a haircut and a shampoo. The stylist left my head hanging in the shampoo bowl too long and when I sat up, I had blurry vision. At first, I thought it might be a cornea problem, but then my vision normalized so I thought everything was okay. The next day, I started to notice that I had numbness on one side of my face and I began to develop a headache."
She was caring for hospitalized patients at the time, and the symptoms remained for several days. "So how does a physician get healthcare? A friend who was a pediatric neurologist met me on a weekend, and he heard the whole story. He was worried about a disease like MS, so I had an MRI. To my surprise they pulled me out of the machine to tell me I had dissected my carotid artery. I was ready to leap out of the scanner anyway...who knew that I was claustrophobic?"
A second MRI confirmed more details of the carotid artery dissection – which is a separation of the layers of the artery wall supplying oxygen-bearing blood to the head and brain. The most serious outcome of this dissection is a severe stroke. "There is actually a name for this condition: beauty parlor stroke syndrome," Dr. Biller notes wryly.
Dr. Biller spent a few days in the hospital and was on anticoagulation medicine for several months. She says that an "aha moment" occurred when several of her male physician colleagues were looking at her MRI images and didn't understand how the dissection could have been caused by getting a haircut. "I realized that this was a bunch of men who just get their hair cut without shampooing, so I had to explain to them the gender differences regarding treatment in the salon. It made me realize that we all have assumptions of what an activity means, and that we have to ask additional questions to understand what exactly was involved – because on this occasion their frame of reference was different than my frame of reference."
Within three to four weeks, some of her symptoms returned. "One of my doctors told me, 'Julie, you are human just like everyone else. You need to take a leave of absence to take time to recover.' That was excellent advice. Healthcare providers try to minimize disruption in their personal lives because of concern for the patients they take care of, but we really need to take time to heal. And going through the experience of allowing time to heal my body was a teachable moment for me – and something that I pass along to my patients: 'Take the time to heal and listen to your bodies.'"
As for other lessons learned, "Being clear about a patient's specific problems comes from my miscarriage experience and was reinforced with my dissection. I want my patients to know the range of what their workup might be, as well as the options for evaluation. I want them to be alert to potential problems that might need to be communicated back to their healthcare team sooner rather than later. Within a reasonable boundary, I will share that I have been hospitalized and that I know it can be scary – but that we will work through it together. I try to give them as much information as possible. I often relate that I have had MRIs and that they were not easy to go through – but the chest scans I order for my patients are a lot less stressful than the MRIs!"
After two decades, Dr. Biller still is very careful about her head placement. "It has worked to my advantage because I've been able to opt out of certain things with my kids – like going on rollercoasters."
Todd Burner, MD
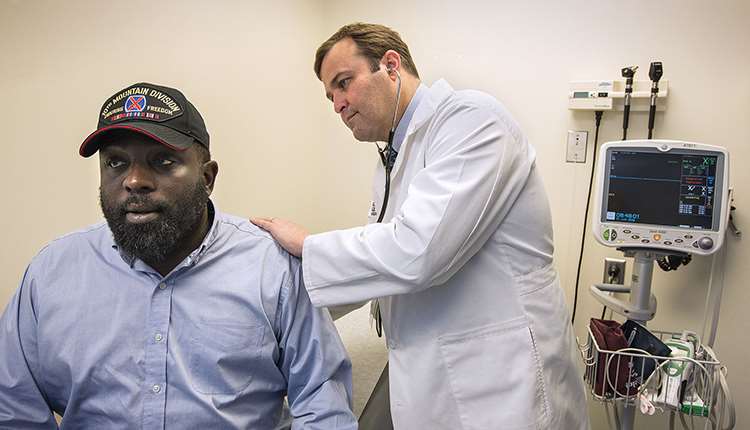
"I was making breakfast for my daughter when I felt this numbness and tingling go all the way down the back of my left leg, and almost immediately it affected my gait. At first I thought it was sciatica, since I had been working out the night before. I finished breakfast and limped into a meeting at MCW – and halfway through the meeting I realized I was going to be hobbling into the ER rather than to my office. It was a long, horrible walk..."
Thus began the arduous journey of Todd Burner, MD '01, GME '04, FEL '08, assistant professor of medicine (rheumatology), who in 2010 contracted Guillain-Barré syndrome (GBS), a rare disorder in which a person's own immune system damages their nerve cells, causing muscle weakness and oftentimes paralysis. GBS can cause symptoms that usually last for a few weeks. The exact cause of GBS is unknown, but it is often preceded by an infectious illness such as a respiratory infection or the stomach flu – and rarely, recent surgery or an immunization.
That first day, Dr. Burner spent a total of 12 hours in the Froedtert Hospital emergency room but physicians were unable to find "the smoking gun" and he was discharged. Later that night he began retaining urine, for which he ultimately had to endure a Foley catheter for many weeks. Follow-up neurological testing revealed GBS, and Dr. Burner was immediately admitted to Froedtert Hospital. During his four-day stay there he was administered four separate infusions of intravenous immunoglobulin (IVig), which, according to Dr. Burner, "binds to the bad antibodies in your system and washes them out and/or neutralizes them."
Following his discharge from Froedtert, Dr. Burner's left leg was still very weak and significantly swollen, and he continued to retain urine. "It was horrible and it didn't get better right away. We did what we could and held our breath. I had two weeks of suffering at home and then came back to work with a cane and the catheter. It was debilitating, but I hobbled around and took care of patients, which was important to me. A month or so later, the catheter was removed, I was improving via physical therapy, and I ultimately bounced back."
Dr. Burner is a rheumatologist who sees patients at the Zablocki Veterans Administration Medical Center in Milwaukee. "I enjoy working with veterans. They are appreciative, and I appreciate the service they have given to our country. It's important for me to try to figure out how I can pay them back in some way."
Dr. Burner's clinical duties are twofold: taking care of hospitalized patients and treating rheumatology patients in the clinic. An interesting twist to this story is that as a rheumatologist, Dr. Burner treats patients with arthritis, autoimmune diseases and pain disorders affecting joints, among other maladies – some of whom require regular infusions of IVig on an out-patient basis.
"My experience with GBS has made me a better doctor, a better communicator. It took my level of empathy to a new high. In the hospital, when I heard my doctor talk to me about things I talk to my own patients about all the time, it was like an out-of-body experience. All of sudden I'm the patient – and he did a great job talking to me. It made me think about how my patients think about the ways I talk to them – which in turn made me think about how I can better communicate to my patients. There is a certain group of them with whom I share my experiences; I tell them a brief version of my story and how it has made me a better doctor – and they appreciate that. It also taught me what it means to be hospitalized, what it does to families, how to discuss illnesses with children. It has made me understand where the families are coming from and helped me to communicate better with them. Without a doubt, it has affected every realm of my practice."
Gabrielle Geddes, MD

"My mother was diagnosed with multiple sclerosis (MS) when I was 12 years old, and over the next few years she was mostly bedridden. I was her primary caregiver, and we had a lot of medical stuff around because she was getting shots and infusions. I learned how to administer injections and through this, I learned a lot about IVs and such – and I found it interesting. But by the time I was in high school, I began to have my own autoimmune health issues, which continue to this day."
Gabrielle Geddes, MD, GME '15, assistant professor of pediatrics (genetics), has been face-to-face with illness and disease since childhood – as both a caregiver and a patient with chronic maladies. "During medical school I started having more significant health issues, including my first episode of optic neuritis – which is an inflammation of the optic nerve often associated with MS. During my internship year, I had another episode. Things got worse, and I was examined by a neurologist who – because I had an abnormal reflex in my hand – told me he thought I had MS. All my scans were negative, and I saw a rheumatologist who started me on an immunosuppressive drug. Then I got septic and was hospitalized."
Dr. Geddes had several more bouts, and at one point was told by a doctor who had not examined her that her condition was "all in her head." Another physician diagnosed her with neuromyelitis optica (NMO), which he said could likely lead to blindness, paralysis and perhaps even death over a five-year period. "This was five years ago, and I’m still here...but I thought I was going to die of this."
"I decided to go ahead with my training in genetics and gained some level of control by telling myself I would kill myself if things got really bad. But they didn't. I still have chronic stuff but nothing severe. I thought: this is what the future holds for me and I am going to be just like my mom. Ultimately, this has made me more dedicated to medicine and more dedicated to my patients, because I thought that whatever time I have left to live, my purpose is to be a doctor. I feel a deep calling that is almost religious. This is my exact purpose in life...that I am here to help, however I can. So I rededicated myself to my work."
Dr. Geddes is now supported by a local excellent care team, including a neuro-ophthalmologist who told her there was no way she had NMO; rather, he diagnosed her with autoimmune optic neuropathy. She also sees rheumatologist David Gazeley, MD, FEL '11.
"The insight that this has given me is that we often are wrong in medicine. That's true in genetics, too. Sometimes in genetics I like being wrong, because I have said a patient would succumb to his/her disease and they didn't. Also, I know how stressful it is to be wrong about those types of things, especially since I am usually talking about children. It has made me more humble; when someone asks me something I am perfectly content with saying, 'I don't know' or 'nobody knows that' or 'let me look to find more information.' It has made me be much more humble about being uncertain about things – and in genetics there is so much uncertainty.
"I also like to think it has given me a bit more compassion. I think in a way, medicine has given me more than I've given it. My specialty is children with congenital heart disease, so if I wake up stiff, and it's hard to move, and I'm in pain, I know there is a kid with one ventricle running down the hallway – so I have to get up and get moving. Ultimately, my patients have given me more than I've given them. I have more ability to cope with the stresses of being chronically ill, and the annoyance of being chronically ill. I am on a teratogenic immunosuppressive drug, so I likely can't have children because they would be born with major birth defects – but my patients are my children, so that's okay. I think that also gives me more insight and empathy when I am talking to people about their reproductive issues."
Mary Horowitz, MD, MS

Twelve years ago, Mary Horowitz, MD '80, GME '85, FEL '89, MS '91, the Robert A. Uihlein Professor of Hematologic Research, was diagnosed with stage IIB breast cancer. A few years later, her husband, Mark, was diagnosed with frontotemporal dementia, a progressive degeneration of the areas of the brain responsible for decision-making, behavioral control, emotion and language. She will quickly point out which one has been more difficult.
"When I was diagnosed, I knew the language and understood what was happening and what I needed to do – and that my chances for survival were good," says Dr. Horowitz, an oncologist and blood and marrow transplant researcher. "But I don't know much about his disease, and what I learned was harder to handle. There is little that can be done, and I can only watch him get worse and worse. I've had 10 years of continual loss."
Each of these experiences has led Dr. Horowitz to different insights about the care she provides.
"I am very comfortable in a hospital and around healthcare providers; I have no clue how patients who aren't oncologists handle this. It can be so scary in a hospital, and people don't process news as fast when they are having emotional reactions." To exemplify this last point, Dr. Horowitz shares that when she went in to receive her diagnosis, she brought along a colleague, and was so glad she did because she didn't remember anything her oncologist said.
"I always thought I was empathetic, but now when I'm with a patient, I talk slower and give them time to process the news and come up with their follow-up questions. I repeat whenever I think it might be necessary and will sit down so they don't feel rushed or flustered. I am always thinking about how the diagnosis and interaction sounds on the other side of the desk."
As a world-class leader in blood and marrow transplant research and scientific director of MCW's Center for International Blood and Marrow Transplant Research, Dr. Horowitz travels quite a bit for work. Her husband now requires daily check-ins, which makes logistics difficult during these trips and has given her a new appreciation for single parents.
"My husband's care gave me much more sympathy for single parents. It can be difficult to balance work with the needs of someone who requires help for his social interaction, and to feel happy and safe. This is the first time in my 40-year career where balancing home life and my career has become difficult for me. When my children were small, my husband shared those responsibilities and they were manageable."
Kenneth Lee, MD

In 2004, Kenneth Lee, MD '93, GME '97, FEL '99, MCW associate professor of physical medicine and rehabilitation, was stationed in Iraq treating his battle buddies who were wounded in the field, when he himself was badly injured by a suicide car bomb. The incident caused traumatic brain injury, post-traumatic stress disorder, and nerve and joint damage that led to years of therapy, surgery and deep, dark depression. The darkness continued until his fellow veterans gave him a renewed sense of purpose.
“We are trained to have a battle buddy. That battle buddy mentality comes out when I am treating a fellow veteran. They are my patients, but they are my comrades as well."
Throughout his rehabilitation – the surgeries, the physical therapy (PT) and occupational therapy (OT), the sessions with the psychiatrist – as well as throughout his own internal battles, Dr. Lee paid attention to what he liked, what he didn't like, and how he felt along the way. These notes paved the way for changes he made to how he interacted with and treated his veteran patients.
As an example, he says he remembers how boring PT and OT were, and how they seemed to drag. So he launched an adaptive sports and recreation league to make therapy more engaging and interesting for his patients. This includes activities such as sled hockey, wheelchair lacrosse and goal ball.
"So many of these paralyzed veterans have it worse than I ever had it, and seeing their resilience and perseverance as they participate in these sporting events helped bring me through my ailments. We help each other. Now, I am enjoying life with my family members and my spinal cord injury veterans, all of whom have saved my life and career."
Dr. Lee's spinal cord injury patients face many of the problems he faced and experience many of the same feelings, and he shares that he helps them as much as he can along the way because he can relate.
"Being a veteran, and having been a patient at the VA, I understand so much about what they are going through. Like when they don’t want to deal with the pain, or are feeling lonely and scared and want to harm themselves. Or when they start wrapping the emotional aspects of their injuries into the physical parts and worry too much about what people think about how their injuries make them look. I can relate on so many levels. The first time I went to the YMCA after my injuries, parents took their children out of the pool because they thought I had a disease.
"We always tell our patients there are support services available to them. Because I have used almost all of them, now I can look my patients in the eyes and tell them with complete certainty those services work. They help. And they believe me because I can talk to them in their own language. And from my experiences, I also try to convey how strong and important family support can be. I want them to understand it gets much easier if they bring others into it."
Dr. Lee also tries to impart lessons he learned onto the medical students and residents.
"It is important for them to know that patients have lives away from what they are being treated for, and that there is life after care. I like bringing students and residents to the adaptive sports events to see the fruits of their work – to see what patients are getting better for."
John and Julie Owen, MD
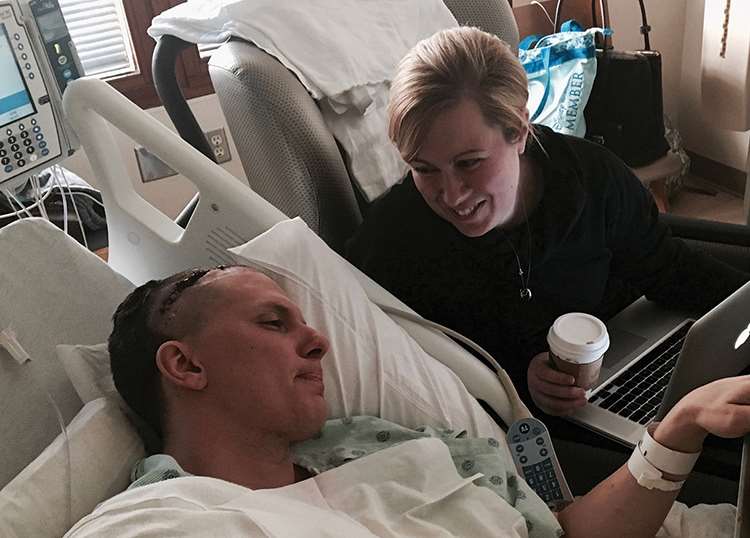
In his third year of medical school, on the last day of his general surgery rotation, current MCW-Milwaukee medical student John Owen woke up in the back of an ambulance. He later found out he had had a massive seizure, which led to work-ups and testing and the eventual diagnosis of an 8cm right frontal tumor. John had brain cancer.
Little did he, or his wife, Julie R. Owen, MD '14, GME '17 (who was a third-year psychiatry and behavioral medicine resident at MCW at the time), know the impact this event would have on their lives and their careers.
Prior to medical school, John Owen had worked as a nurse in the Froedtert Hospital emergency department for four years while Julie went through medical school at MCW-Milwaukee. He and his wife have had plenty of opportunity to interact with patients. But, as they both say, those interactions will be different going forward.
"Being a patient will make me a much slower doctor. I had no idea what it was like for many patients before I became one," he says. "I'm much more accepting of a whole variety of presentations. Whether patients come in and they are grumpy, or tired, or not engaged or not motivated, I've felt all of those, so I can appreciate them. I'm much slower to judge than I ever was before. I'm ashamed to say that."
Dr. Julie Owen adds, "I know what suffering feels like. I know what challenging situations feel like. Having that firsthand experience impacts how I treat patients. Having gone through this with John, I have cultivated a deeper sense of empathy for others. I'd like to think I always had it, but it has definitely grown after being on the patient side of things."
The Owens agree that their chosen careers made going through this both easier and more difficult.
"I am thankful for the additional understanding of what is going on and what is involved, and for knowing the physicians who cared for me," John Owen remarks. "But I also know all of the other possibilities. I've cared for people whose experience with brain cancer didn't go well, and it's not a pretty sight. Thinking about that for myself was very difficult."
Dr. Julie Owen echoes those sentiments. "The perspective you have as a physician is so valuable when you are thinking about your own situation, but the knowledge base – what the data and research indicate – can be difficult to overcome."
John Owen had to extend his medical school training by one year because of the treatment, but has no regrets. MCW developed a plan to allow him to graduate on time, but it would have required him to give up all his electives, some of which he needed to go into emergency medicine – which is a trade-off he wasn't willing to make.
Having gone through this, he has a new perspective he likes to share. "Before, I approached my life with the assumption I had 80 or 85 years. But now, I realize I may never get a 'later'; later may never come. You have no idea what people are going through when they see you in the store, or make a disparaging gesture. We need to give people more credit. Give people more slack. No matter what your problem is that day, others have it worse."
Iris Kassem, MD, PhD
Seeing your son have six-hour "nosebleed bloodbaths" year after year can be difficult, but for Iris Kassem, MD, PhD, the worst part was seeing the impact it had on Ryan. He was afraid to go to sleep because he worried he wouldn't wake up when the bleeding started, and he'd choke to death. Dr. Kassem had a hunch there was more to Ryan's condition than what his physicians were indicating, and she turned out to be right.
Ryan went to Joseph E. Kerschner, MD '90, FEL '98, professor of otolaryngology and communication sciences, for the nosebleeds, and, as part of his work-up, was enrolled in a clinical trial at the BloodCenter of Wisconsin. It turns out Ryan has a genetic disorder, von Willebrand disease, which prohibits his blood from clotting properly. Ryan now has an inhaler that will help his blood clot in fewer than 10 minutes, which allows the active 11-year old to confidently sleep and even play goalie on the Milwaukee Jr. Admirals.
The hunch Dr. Kassem carried with her throughout Ryan's testing has impacted how she sees patients. "I listen to the parents of my patients a lot more," says Dr. Kassem, who is a pediatric ophthalmologist and researcher. "If they feel something isn't right, I trust their instincts. I had a similar feeling for a while, and it doesn't fail me to listen to parental instincts."
Dr. Kassem's research focuses on pediatric cataracts, retinopathy of prematurity and improving visual outcomes. While going through all of Ryan's testing, she started to notice that some complications of the eyes have similar complications associated with von Willebrand disease, and she now focuses part of her research on finding more of these connections. It is her way of connecting her personal and professional efforts.



