Serving Those Who Serve
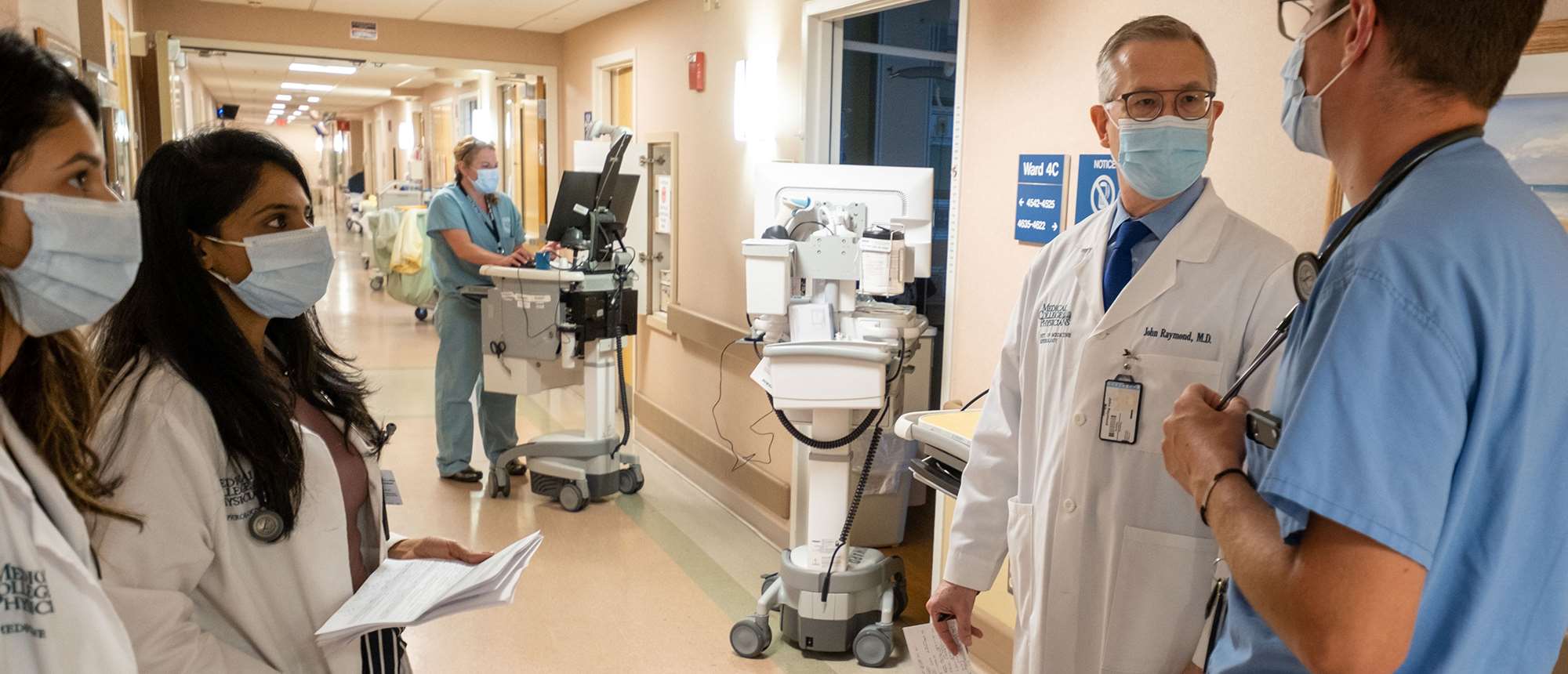
The 76-year partnership between MCW and the Zablocki VA Medical Center benefits both doctors and patients
When the predecessor institutions of the Medical College of Wisconsin (MCW) and the Clement J. Zablocki Veterans Affairs Medical Center created their partnership in 1946, the primary goal was to provide enough physicians to meet the medical needs of the millions of Americans returning from World War II.
More than seven decades later, the collaboration continues to further the missions of both entities by offering cutting-edge care for veterans and their families and enriching the professional development of medical students, residents, interns and fellows. Support for this collaboration starts at the very top of MCW.
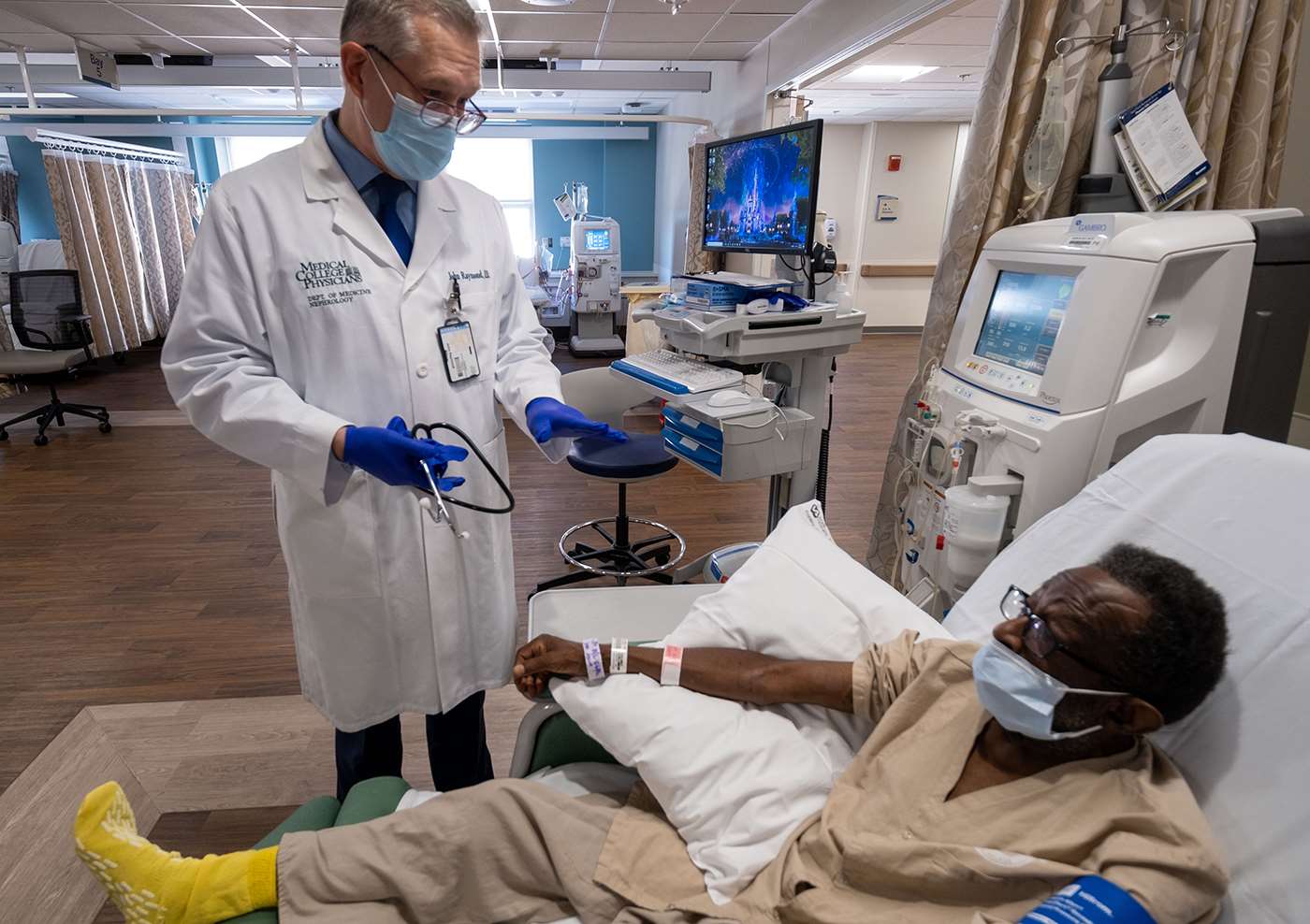
Treating veterans has long been a passion for John R. Raymond, Sr., MD, president and chief executive officer of MCW. A practicing nephrologist, Dr. Raymond served for seven years as a section chief treating patients with renal failure at the Durham Veterans Administration Medical Center in Durham, North Carolina, early in his career. Since becoming president and CEO of MCW in 2010, he has served a clinical rotation each August at the Zablocki VA Medical Center in Milwaukee.
“The Durham VA was exceptionally busy,” Dr. Raymond recalls. “At any one time, I could be responsible for 100 renal transplant patients and 150 home dialysis patients. Those experiences honed my skills as a physician and forged a lifelong commitment to veterans and patients with renal diseases.”
“Even as I worked to expand my own research and took on administrative duties throughout my career,” Dr. Raymond adds, “I always strove to maintain a robust array of clinical duties.”
The reason? “For me, patient care brings meaning to my nonclinical duties,” he says.
“The VA is an incredible learning resource for medical students,” says Jon Lehrmann, MD, the Charles E. Kubly Chair in Psychiatry and Behavioral Medicine and professor and chair of the Department of Psychiatry and Behavioral Medicine. Dr. Lehrmann also serves as associate chief of staff for mental health at the Zablocki VA Medical Center. “Part of my training was at the Milwaukee VA,” Dr. Lehrmann notes.
According to statistics from the US Department of Veterans Affairs, the VA is the largest healthcare training system in the country, providing training, residencies, and fellowship to more than 120,000 healthcare students in more than 60 disciplines each year.
“The missions of the VA and MCW align,” Dr. Lehrmann adds. “The VA values education, and by working with the VA, MCW improves the health of the communities we serve. And one of those communities is veterans.”
One outstanding example of the two organizations working together to help veterans is The Captain John D. Mason Veteran Peer Outreach Program, which aims to prevent suicide by connecting veterans to mental and physical healthcare at the VA. Captain John D. Mason was a Vietnam veteran who died after a long struggle with depression and post-traumatic stress disorder (PTSD). Mason’s best friend, Joe Tate, made a gift to MCW to create the program.
“The Captain Mason program is housed at MCW, but the peer outreach is done by veterans at the VA who have experience with mental health issues,” Dr. Lehrmann explains. “They go into the community and help veterans get into the VA system. Veterans have a higher risk of suicide than the average person.”
Susan Tsai, MD, MHS, FACS, Douglas B. Evans Chair for Surgical Research, professor of surgical oncology and director of the LaBahn Pancreatic Cancer Program has been treating patients at the Zablocki VA Medical Center for the last 12 years.
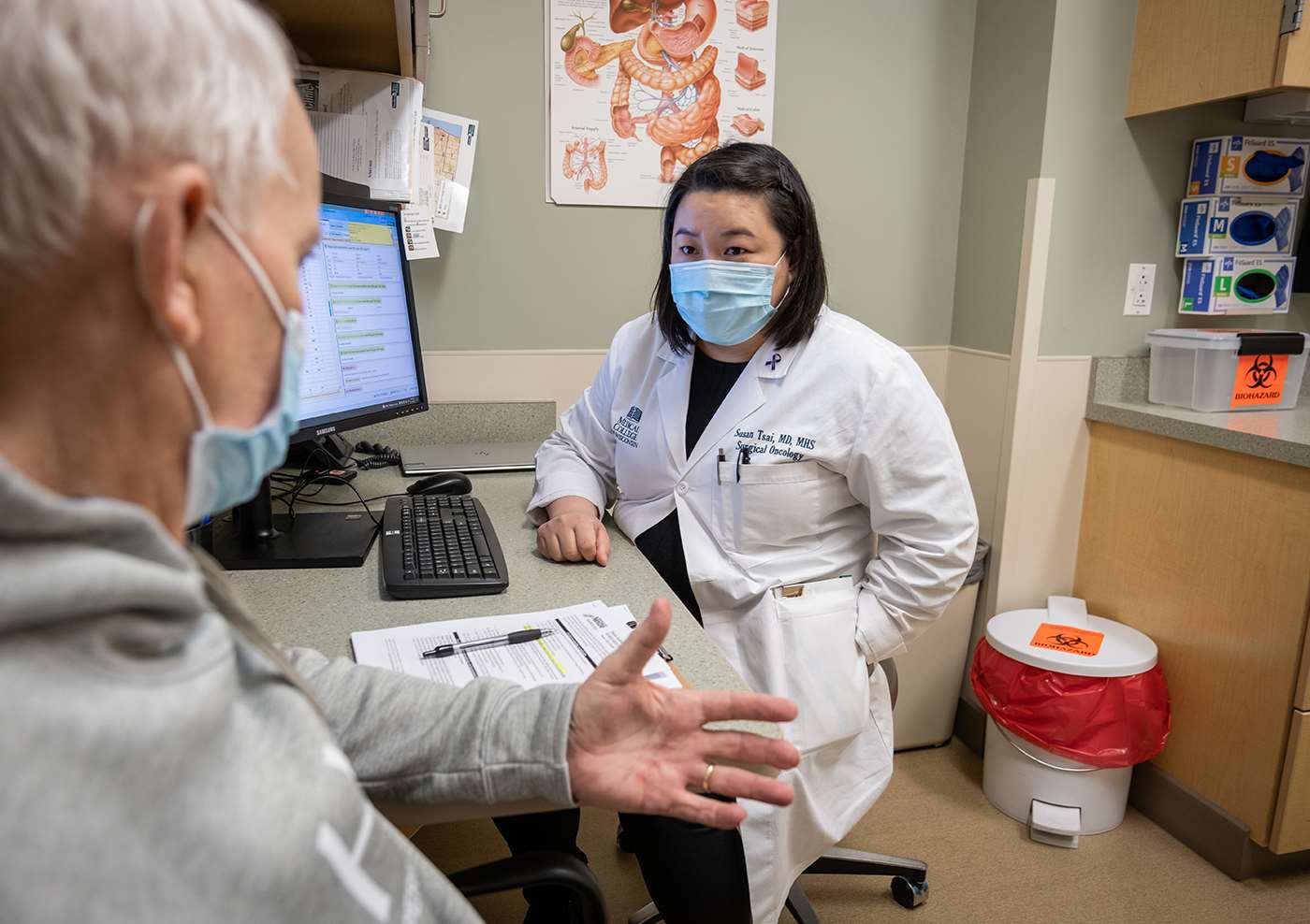
“For the patients I see at MCW, they often don’t have the same social support needs – food and housing insecurity, for example – that the veterans do,” Dr. Tsai says. “When veterans are facing these social inequities, delivering treatment for a very serious cancer like pancreatic cancer can be very challenging. For anyone diagnosed with pancreatic cancer, the diagnosis itself is challenging and the treatment is a whole other level on top of that. Treatment is not just one modality, it’s surgery and chemotherapy and radiation combined. The cumulative effect of the treatments can be very taxing, emotionally, financially and socially.”
Dr. Tsai notes that the VA offers support for veterans including transportation, housing, food, and other needs. This ensures that no one goes through the diagnosis and treatment alone and allows the veteran to focus on the cancer and its treatment.
“What I can share from MCW to the VA is cutting-edge treatment for pancreatic cancer,” Dr. Tsai says. “And what I learn from the VA going back to MCW is how to care for the underserved because I think the VA does that really well.”
Both Dr. Tsai and Dr. Lehrmann agreed that working at the VA is a way for them to give back to, and honor, those who serve in the military.
“My father was an Army paratrooper,” Dr. Lehrmann says. “I have an emotional commitment to serving veterans. It’s part of my life’s mission.”
“I think it’s everyone’s desire at MCW to engage in community outreach and serve the community in which we live, and veterans are an integral part of that,” Dr. Tsai adds. “They deserve the best care. I think that’s why so many people love to work at the VA. It’s such a pleasure to take care of veterans. Not only are they very appreciative, but they have made sacrifices that most of us can’t say that we’ve made. It’s a privilege to care for them.”



