MCW APP Adult Critical Care Fellowship Program
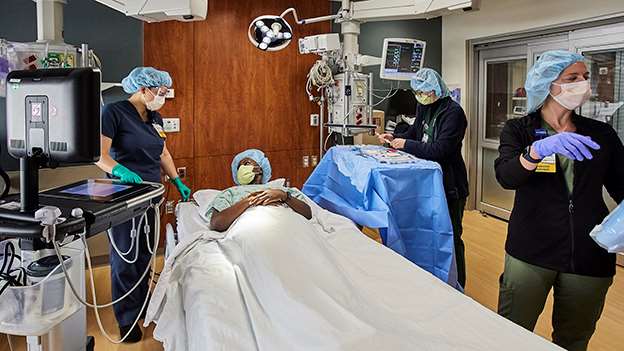
Who should consider an APP critical care fellowship?
APPs with interest in advancing their clinical skills to assess, diagnose, and treat complex, critically ill patients.
APPs interested in transitioning to practice in a mentored environment to build a professional network and clarify through experience a best fit for clinical practice and starting their career.
What are the benefits of an APP critical care fellowship?
Hands-on learning and time to develop competency and confidence needed to thrive in an intense, diverse and complex environment.
Structured experiences targeted to new graduates or APPs transitioning to a new practice area.
Mentored learning in clinical rotations across six (6) ICUs and in specialty rotations.
Provides the opportunity to develop a wide range of clinical and critical thinking skills and professional development with application across diverse clinical specialties.
Apply to the APP Adult Critical Care Fellowship Program
Fall and Spring start dates are available; up to 4 fellows are selected annually, split between cohorts.
Learn more about application details, including information about interviews, salary, and benefits.
A Day in the Life of an APP Adult Critical Care Fellow
Clinical Rotations
Acute Care and Mini-Rotations
Fellows can expect a traditional 8 a.m. - 5 p.m., Monday-Friday schedule during these rotations. These rotations serve to enhance the fellow experience through exposure to consultative and procedure-based services, team structures and workflows, and specialty knowledge acquisition.
ICU Rotations
Each day, APP Fellows work in conjunction with an APP preceptor to care for a panel of 3-6 critically ill patients. APP Fellows are integrated into the academic, multi-professional critical care team. Fellows can expect to work 13-hour shifts with variable start times by rotation, work both day and night shift and some weekends.
ICU Day Shift
- 0630: Arrive in the ICU team room, confirm patient assignments and receive hand off from the night provider.
- 0700-0800: Pre-rounding. Review data, assess your patients, and discuss any updates with the bedside nurse. Prepare for rounds, formulate a plan of care for the day, and discuss questions with APP preceptor.
- 0800-1100: Academic critical care team rounds. Active participation in academic patient care teaching rounds for all patients on the critical care service. APP Fellows are expected to orally present patients to the multidisciplinary team and collaborate with the critical care team to facilitate workflows and patient management. Patient-based, hands-on bedside teaching by the critical care team.
- 1100-1900: Critical Care Management. APP Fellows provide ongoing assessment and management of their patient panel, including writing critical care notes, completing procedures, following up on changes in patient condition and updating patients and their families. APP Fellows work within the team to transfer, discharge and admit patients throughout the day. APP Fellows attend service-based education as appropriate. At the end of shift, APP Fellow provides hand off to the night provider.
ICU Night Shift
APP Fellows work in conjunction with APP preceptor to care for and manage 8-12 critically ill patients. Night workflows include providing active management of patients including rounding and cross-coverage needs, admitting new patients, and performing necessary procedures. Night shift provides unique opportunities for hands-on management, individualized teaching, and close collaboration with critical care APPs and intensivists.
Didactic Education
Education/Program Days
Scheduled 2-3 times per month, full (8 a.m. - 4 p.m.) or half days on campus with all program fellows dedicated to didactic education, program meetings and fellowship connection. Schedule varies by day, but may include expert lead chalk talks, simulations and skills labs, case-based learning, peer lead curriculum including fellowship scholarly journal club, case presentations and point of care ultrasound and professional and leadership development curriculum. Additionally, program meetings including program touch bases, quarterly reviews and mentorship meetings may be scheduled. Finally, fellows have time to complete asynchronous education and work on their fellowship projects.
How We Learn
The APP Adult Critical Care Fellowship Program focuses on hands-on, clinical experiences across all six (6) ICUs in addition to key acute care specialties as the foundation for critical care practice. In addition to clinical rotations providing patient experiences across each specialty ICU, the core critical care curriculum provides continuity and skill development focusing on 15 aspects of essential critical care skills throughout the 12-month program.

Featured Voices

"I decided to pursue an APP Fellowship to gain additional critical care experience, explore new areas of critical care and to ease my transition into practice as a new graduate. In addition, I was seeking procedural experience and wanted to learn and grow as a provider in a supportive environment. I thought MCW would be a great place for me to start out my career as a critical care APP because it is an academic medical center & quaternary care facility with five specialty ICUs and level 1 trauma designation. I also went to school at Marquette and was hoping to stay in the Milwaukee area after graduation."
Keighla Slattery, MSN, APNP, ACNPC-AG, CCRN

"I wanted to gain confidence and critical care skills in an intensive, supportive environment where I would be exposed to diverse patient populations and practice styles. I was drawn to Froedtert Hospital which, as a level one trauma center with five intensive care units, serves some of the most complex patients in and around Wisconsin. It is also a very APP-focused institution. The APP fellowship was instrumental in shaping my practice; it gave me confidence as a critical care provider, experience with varied patient populations, and skills for working on complex, multidisciplinary teams."
Laura Mark, PA-C, MPH
Current Fellow

Ryan Bohara, APNP
Adult Critical Care APP Fellow
Meet Our Program Team
Education for the APP Adult Critical Care Fellowship program is supported by an APP, MD, and education coordinator leadership team in addition to APP and MD specialists and educators from all critical care specialties and key acute care rotations. Current and past APP fellows enhance the fellowship team through their commitment to learning and engagement.

Kaitlin Spiegelhoff, MPAS, PA-C
Physician Assistant
MCP Advanced Practice APP Critical Care Fellowship Program Manager

Thomas Carver, MD, FACS
Professor, Medical Director SICU
APP Critical Care Fellowship Physician Program Director


Michelle Washburn, BA
APP Adult Fellowship Program Coordinator
Contact Us
For general fellowship questions or to submit additional application documentation
appcriticalcare@mcw.edu

