Medical College of Wisconsin Pediatric Critical Care Fellowship Program
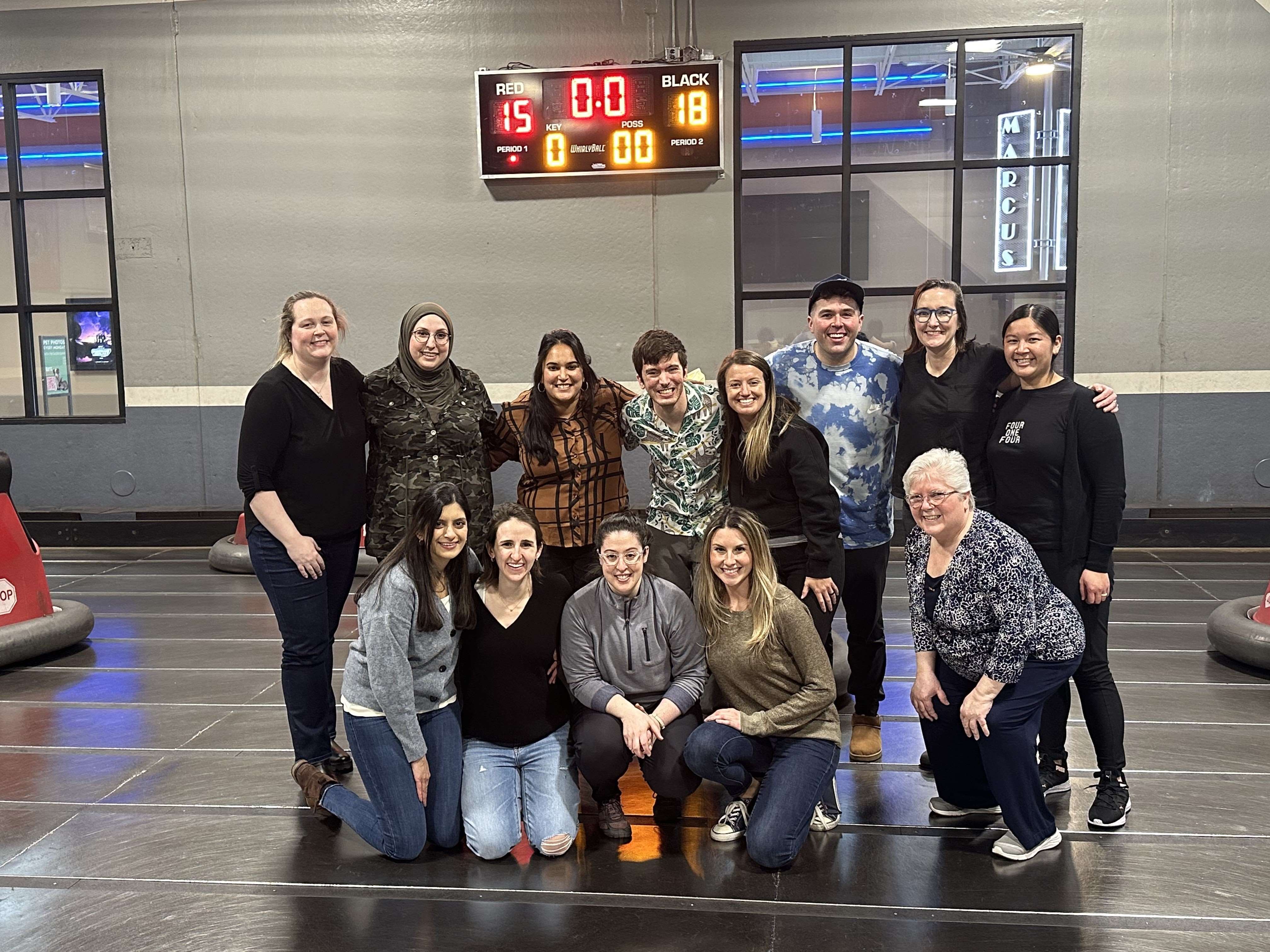
A Message from Our Program Director
 As program director, it is my honor to develop and train the next generation of physicians, researchers, and leaders in pediatric critical care medicine. Our program is dedicated to providing our fellows with a broad and intensive clinical experience, a rigorous academic curriculum, and strong foundation in research. Our training will provide the all the skills necessary to set our fellows up for a successful career wherever they choose to go after training.
As program director, it is my honor to develop and train the next generation of physicians, researchers, and leaders in pediatric critical care medicine. Our program is dedicated to providing our fellows with a broad and intensive clinical experience, a rigorous academic curriculum, and strong foundation in research. Our training will provide the all the skills necessary to set our fellows up for a successful career wherever they choose to go after training.
Hilary Schreiber, MD, MA
Director, Pediatric Critical Care Fellowship Program
Pediatric Critical Care Fellowship Tour
As a Pediatric Critical Care fellow you will...
- Learn to care for patients with a full spectrum of critical illness including medical and surgical cardiac disease, mechanical support (ECMO, VAD, CRRT), solid organ transplant, bone marrow transplant, oncologic diseases, neurologic and neurosurgical diseases, and other medical and surgical diseases
- Learn to provide critical care consultation and remote management for patients in referring institutions as a member of our critical care transport team and medical control
- Participate in protected critical care educational conferences
- Identify your personal scholarly interest(s) with close mentorship from faculty
- Attend and ideally present your research at regional or national conferences
- Develop your skills teaching patients, families, medical students, residents, and nurses
About Our Institutions
Medical College of Wisconsin (MCW)
The Medical College of Wisconsin brings together the most inquisitive minds in science, medicine, education and community engagement to solve the toughest challenges in health and society today. Academic medicine is at the core, where scientists, physicians and students work hand-in-hand with the community to ask the questions no one else is and fuel the continuous cycle of knowledge that’s shaping the future of medicine.
Children’s Wisconsin
Children’s Wisconsin is the region’s only independent health care system dedicated solely to the health and well-being of children. We offer a wide range of care and support for children of all ages. Our services include medical care, dental care, child and family counseling, foster care, adoption, social services, child advocacy and injury prevention.
About Our Fellowship
Our Fellowship in Photos
Our Spaces & Places
I find immense value in the ability to work as a multidisciplinary group within the PICU. Our institution has many great minds and leaders in their respective fields. The opportunity to have an open and collegial discussion with other subspecialties regarding not only patient care but ongoing research and education has been instrumental in my growth and development as a fellow. There is a great respect for the fact that our hospital is a teaching institution on many levels and faculty take every opportunity to teach and mentor trainees.”
A former Fellow
Current Fellows

Hanna Distel, MD
Pediatric Critical Care Fellow, 2023-2026
Medical School: University of South Dakota, Sanford School of Medicine; Residency: University of Hawai'i

Hollis Johnson, MD
Pediatric Critical Care Fellow, 2023-2026
Medical School: Medical College of Wisconsin; Residency: Spectrum Health/Helen DeVos Children's Hospital

Lucia Bracco, DO
Pediatric Critical Care Fellow, 2024-2027
Medical School: University of Pikeville - Kentucky College of Osteopathic Medicine; Residency: Advocate Children's Hospital Park Ridge IL

Tony Chuang, MD
Pediatric Critical Care Fellow, 2024-2027
Medical School: University of California, Irvine, School of Medicine; Residency: Mayo Clinic

Ryan Grammens, DO
Pediatric Critical Care Fellow, 2024-2027
Medical School: Pacific Northwest University of Health Sciences College of Osteopathic Medicine; Residency: University of New Mexico

Bianka Martinez, DO
Pediatric Critical Care Fellow, 2024-2027
Medical School: Burrell College of Osteopathic Medicine at New Mexico State University; Residency: University of Illinois at Chicago Pediatrics Residency Program

Katie Mutke, MD
Pediatric Critical Care Fellow, 2024-2027
Medical School: University of Nebraska College of Medicine; Residency: Indiana University

Cassie Mejia, MD
Pediatric Critical Care Fellow, 2025-2027
Medical School: Medical College of Wisconsin; Residency: Medical College of Wisconsin Affiliated Hospitals; Pediatric Cardiology Fellowship: Medical College of Wisconsin Affiliated Hospitals

Adnan Ahmad, DO
Pediatric Critical Care Fellow, 2025-2028
Medical School: Midwestern University Chicago College of Osteopathic Medicine; Residency: University of Wisconsin-Madison

Emily Allen, DO
Pediatric Critical Care Fellow, 2025-2028
Medical School: Kansas City University College of Osteopathic Medicine; Residency: University of Louisville

Miguel Pareja Cajiao, MD
Pediatric Critical Care Fellow, 2025-2028
Medical School: Colegio Mayor de Nuestra Senora del Rosario Facultad de Medicina; Residency: BronxCare Health System

Erin Whiteford, MD
Pediatric Critical Care Fellow, 2025-2028
Medical School: Creighton University School of Medicine; Residency: Medical College of Wisconsin Affiliated Hospitals

Glory Ayanda, MD
Pediatric Critical Care Fellow, 2026-2029
Medical School: Windsor University School of Medicine; Residency: Corewell Health William Beaumont University Hospital
Nisha Karwal, DO
Pediatric Critical Care Fellow, 2026-2029
Medical School: Kansas City University College of Osteopathic Medicine; Residency: Washington University/St. Louis Children’s Hospital

Swathi Menon, MBBS
Pediatric Critical Care Fellow, 2026-2029
Medical School: Smt. Kashibai Navale Medical College and Hospital; Residency: Icahn School of Medicine at Mount Sinai/NYC Health and Hospitals (Elmhurst) Program
Neha Muthavarapu, MD
Pediatric Critical Care Fellow, 2026-2029
Medical School: St. George’s University School of Medicine; Residency: University of Illinois College of Medicine Peoria
Hira Rohail, MD, MPH
Pediatric Critical Care Fellow, 2026-2029
Medical School: St. George’s University School of Medicine; Residency: Advocate Children’s Hospital – Park Ridge
Our Team

Hilary Schreiber, MD, MA
Assistant Professor; Director, Pediatric Critical Care Fellowship Program

Rachel Ashworth, MD
Assistant Professor; Associate Director, Pediatric Critical Care Fellowship Program

Jasmine C. Dowell, MD
Associate Professor; Associate Director, Pediatric Critical Care Fellowship Program

Adam O. Szadkowski, MD
Assistant Professor; Associate Director, Pediatric Critical Care Fellowship Program

Hayley Severson, MLIS
Education Program Coordinator II

Angie Koepke
Administrative Assistant Sr.
Contact Us
Thank you for your interest in our program. We look forward to connecting with you!
Department of Pediatrics Critical Care
9000 W. Wisconsin Ave. MS 681
Milwaukee, WI 53226
Hayley Severson, MLIS
Fellowship Program Coordinator
hseverson@mcw.edu































