MCW-MKE Psychiatry Residency Curriculum & Rotations
General coursework and rotation information for the MCW-MKE Psychiatry Residency Program.
In this program, you will get therapy training far beyond that which is offered at most other programs. Even if you don’t want to do therapy in your profession, what you learn will make you a better clinician in any area.
Courses & Seminars
Clinical Rotations
The division of the inpatient rotations between the PGY 1 and PGY 3 years is rare among training programs. We believe having experienced residents returning to the inpatient service provides an added dimension to patient care and to teaching medical students.
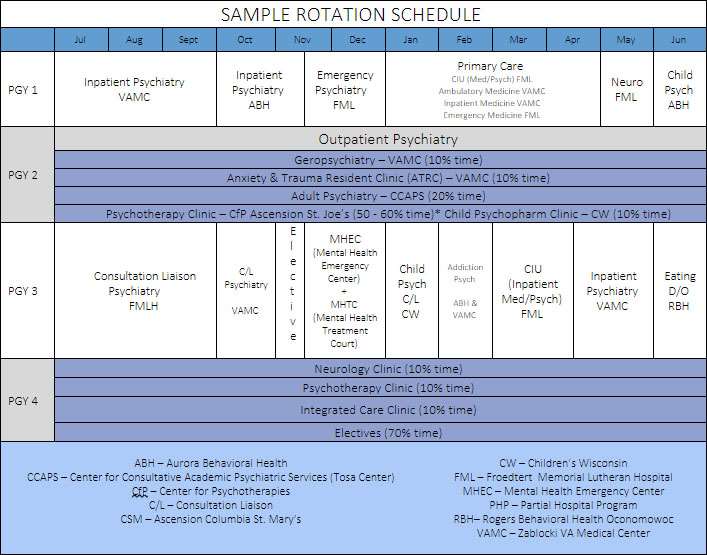
Rotation Details
PGY 1
Half of the PGY 1 class begins on medical rotations while the other half begins with psychiatry. Three-month block rotations permit those residents who started on internal medicine to begin psychiatric rotations in October and vice versa. Hence, the maximum consecutive time away from psychiatry during the first year is three months. Didactic course work is reserved for Wednesday mornings and an experiential support group meets biweekly throughout the first year. Our primary care months include 2 months of inpatient internal medicine, one month of emergency medicine and one month of ambulatory medicine. PGY 1 residents begin Child & Adolescent Psychiatry in their first year, allowing for early exposure to those considering further specialization.
PGY 2
In PGY 2 year, residents move to outpatient psychiatry where they solidify knowledge around diagnostics, medications and psychotherapies.
There are some variations with additional options of Child Psychiatry clinic, North Hills Geropsych Clinic and Sixteenth Street Clinic, but most residents spend one day in the CCAPS (Center for Consultative Academic Psychiatric Services) Clinic at the Tosa Center. This is a general adult outpatient clinic caring for patients referred through Froedtert Hospital or Froedtert Primary Care doctors. One day per week is at the VAMC where residents spend half a day weekly in the geropsychiatry clinic and a half day in the Anxiety and Trauma Clinic.
Half of the week is at the Center for Psychotherapies where residents practice various forms of psychotherapy. In addition to the Wednesday morning didactics, there is a half day of Friday morning didactics in second year focused specifically on many different forms of psychotherapy. Starting outpatient psychiatry in the PGY 2 year allows residents to follow patients for up to three years in their continuity clinics in the 3rd and 4th years.
Additionally, four residents will have the opportunity to rotate at Children's Wisconsin Child and Adolescent Psychiatry Resident Clinic. (Two residents alternating every other Thursday; alternate Thursdays are at the Center for Psychotherapies). This is a new resident clinic at CW on Thursdays where residents will see child and adolescent psychiatric patients that have been referred from Children’s Wisconsin physicians.
PGY 3
The division of the inpatient rotations between the PGY 1 and PGY 3 years is rare among training programs. We believe having experienced residents returning to the inpatient service provides an added dimension to patient care and to teaching medical students. With more psychiatric knowledge and teaching skills later in training, PGY3 residents return to the Complexity Intervention Unit (CIU) at Froedtert Hospital for 1.5 months to serve as the psychiatric leader of the team and provide medical student teaching.
Another 1.5 months are spent on the Inpatient Psychotherapy rotation at the VA Medical Center. On this rotation, residents return to the inpatient unit at the VA and get significant experience leading groups. The one-month Addiction rotation combines experiences at the VA Medical Center with additional day treatment and residential experiences at a private hospital. The PGY 3 residents do one month of Child Psychiatry Consults at Children’s Wisconsin. Four months are spent on the Consultation Liaison (C/L) service. Three of those months are at Froedtert Hospital, a level 1 trauma center and teaching hospital, and one is at the VA Medical Center.
The Mental Health Emergency Center is a 1.5 month rotation for PGY 3 residents. Evenings and nights are the busiest times with the best opportunity for learning. Residents do 10-hour shifts on four nights per week. During this rotation, residents also have the opportunity to participate in Milwaukee County’s Mental Health Treatment Court (a voluntary program designed to enhance public safety and reduce recidivism of those who suffer from serious or severe and persistent mental illness). Residents will evaluate potential participants for the program and provide consultation to the program staff.
PGY 3 residents work on the Eating Disorders Rotation at Rogers Behavioral Health, one of the nation’s leaders in eating disorder treatment. Finally, PGY 3 residents have half of a month of elective time.
Throughout the year, residents continue their half day psychotherapy continuity clinic.
PGY 4
The PGY 4 year is viewed as a bridging and transitional year. In addition to clinical duties, the resident assumes greater responsibility for teaching, supervising, administration, and if desired, research. PGY 4 residents work in an Integrated Care Clinic (embedded in Primary Care), providing consultation to our primary care colleagues. The resident continues with long term outpatient therapy patients and completes the second required month of neurology either through outpatient clinics or on the neurology consult service. Electives provide an opportunity for more intensive work in a myriad of clinical programs.


