A New Key to Brain Surgery
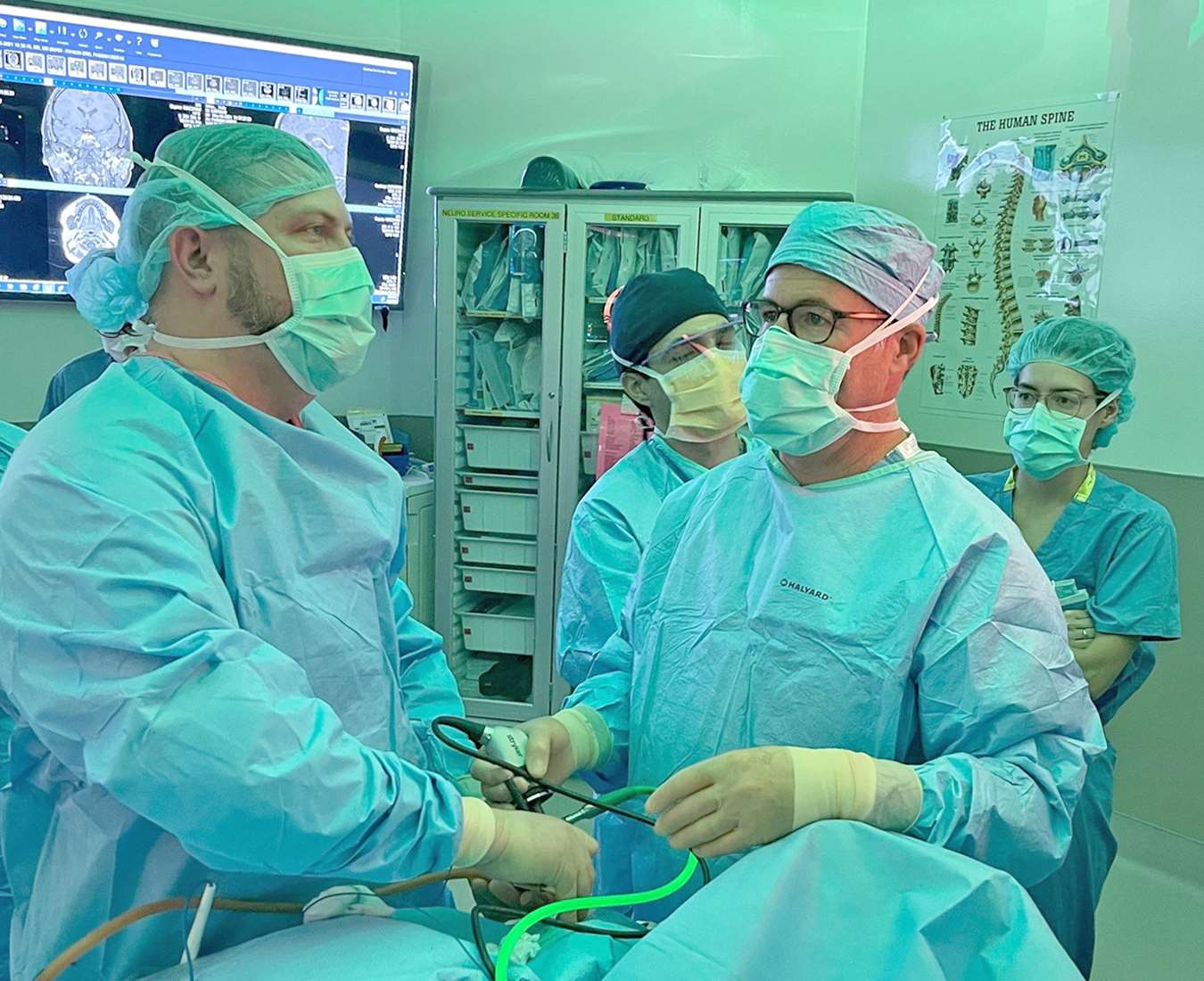
(l-r) Dr. Nathan Zwagerman and Dr. Christopher Michael Long perform a transnasal keyhole surgery.
Receiving a diagnosis where brain surgery is a part of the treatment plan can be one of the most terrifying moments of a patient’s life. A thousand different images of panic, and even hopefulness of a healthy outcome, may flood their mind. Yet it is in these swirling and emotional moments when Nathan Zwagerman, MD, director of pituitary and skull base surgery at MCW, often meets his patients for the first time.
“Every patient I meet is scared,” says Dr. Zwagerman. “There is fear with diagnosis and seeing an MRI with a lesion on it. But my focus is on patient outcomes and laying out a plan for them so they understand what their path is going to look like.”
Dr. Zwagerman specializes in skull base surgery, which addresses tumors around the head band area, typically working between the bone and brain as well as in the fluid-filled spaces within the brain. Patients, often fearing the worst when imagining brain surgery, may be surprised to learn they could be a candidate for a novel and less invasive surgical approach called “keyhole surgery.” Keyhole surgery uses smaller, more direct, nontraditional pathways to perform brain surgery – such as the nose, a crease in the eye, or behind the ear. This can have an immense impact on recovery time and overall response to tumor removal.
“Keyhole surgeries are small approaches to get to a very deep area of the brain. What makes it challenging is that we use different tools to do this,” Dr. Zwagerman remarks. “Traditionally, neurosurgery is done with a microscope, shown in 3D, but you need a wider entry point for that tool to work. For keyhole surgeries we use endoscopes, which provide a wider view from a smaller entry space, but are shown in 2D, and that can be difficult.”
A very limited number of neurosurgeons specialize in this method, which, according to Dr. Zwagerman, is due in large part to the technical difficulty. Dr. Zwagerman, however, has performed more than 500 keyhole brain surgeries during his career.
Dr. Zwagerman says compared to a craniotomy, keyhole surgery patients tend to heal faster and have a shorter hospital stay. The less-invasive approach has cosmetic benefits as well. “Day one after keyhole surgery, patients can look in the mirror and see themselves. They don’t see a shaved head or a scar, and they don’t necessarily look like they’ve just had a big surgery,” Dr. Zwagerman notes.
Due to the involved nature of keyhole surgeries, Dr. Zwagerman works closely with a comprehensive team at MCW, including otolaryngologists, otologists, oculoplastic surgeons and endocrinologists. This comprehensive approach allows each team member to provide their area of expertise, leading to better outcomes.
“This is a paradigm shift, allowing our teams to find new corridors, improve our tools, and better our understanding of brain anatomy and neurosurgery as a whole,” Dr. Zwagerman says. “The standard for brain surgery used to be big operations and craniotomies, but now in some cases we can provide options that critically alter how a brain tumor diagnosis impacts a patient’s life.”
Dr. Zwagerman and his team in the department of neurosurgery are uncovering new findings through research in robotics, tumor genetics and through MCW’s tumor bank. Dr. Zwagerman is passionate about continuous improvement of his craft, including keyhole surgery, as a means to find better ways to take care of people.
“We are hoping to establish a skull base fellowship here at MCW,” notes Dr. Zwagerman. “There are more than 3,000 neurosurgeons across the country, but so few of us know how to do keyhole surgery. Specialized training will help us provide a full range of options to patients.”
– Hannah Thulin



