Medical College of Wisconsin Pulmonary Function Testing
Pulmonary function tests (also called lung function tests) help measure how well your lungs are working. The tests measure the amount of air you breathe out (exhale) and how long it takes for you to exhale completely. These tests are done to diagnose lung conditions such as asthma and COPD. They may be done before and after you take certain medications. They may also be used to find out whether your shortness of breath gets worse with exercise. Over time, pulmonary function tests can help you and your healthcare providers see how well your treatment is working.
About the Test
A complete pulmonary function test has three parts. You may be given the entire test or only certain parts. The entire test is painless and can last 45–90 minutes. If you get tired, you can take a break between test sections.
Before Your Test
Follow any instructions you are given to prepare for the test. Otherwise, your test may be canceled.
- Avoid smoking for 12–24 hours before the test or stop as directed.
- Stop taking your breathing medication 6 hours before the test.
- Avoid caffeine and eat only a light meal. Also, limit the amount of fluids you drink.
- Wear loose clothes that don’t restrict your breathing.
Tell the healthcare provider if you have any of these symptoms during the test:
- Sore mouth
- Chest, arm, or jaw pain
- Fatigue or dizziness
- Severe shortness of breath
During Your Test
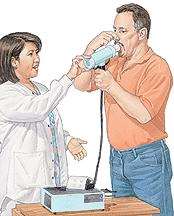
The healthcare provider will coach you during your test. Depending on how many parts of the test you have, you may sit in a chair and breathe through a mouthpiece. Or you may sit in a clear plastic box that looks like a phone booth. You will wear nose clips so you only breathe through your mouth.
- During spirometry, you hold your breath and blow it out fast. Spirometry is repeated at least 3 times to measure your best effort. Spirometry measures how much air you can take into your lungs and how fast you can blow the air out.
- During diffusion, you hold your breath for 10 seconds. The test measures how well your lungs move air into your blood.
- During lung volume, you breathe in different mixtures of air. How much air you inhale and exhale is measured. The amount of air that stays in your lungs is also measured.
- During arterial blood gases, a small sample of blood is taken from a blood vessel (artery) in your wrist. The amount of oxygen, carbon dioxide and hemoglobin are measured.
- During methacholine challenge, you will be asked to inhale, via a nebulizer, increasing concentrations, up to 5 levels, of a medication (methacholine). After each level you will be asked to perform a spirometry test. This test is used to help diagnose bronchial hyperreactivity (asthma), and is also known as a bronchial challenge test.
- 6-Minute Walk, you will be asked to walk, at your normal pace, in the corridor for up to 6 minutes. Before and after the walk, your oxygen saturation (percent hemoglobin carrying oxygen) and heart rate will be taken using a non-invasive monitor (pulse oximetry) attached to your finger.
After Your Test
After the test, you can return to your normal diet, activity, and medications. If you were asked to skip medications before the test, ask if you should take them now. Your doctor will discuss the test results with you at your next visit.
Words You May Hear
Pulmonary function tests measure how much air you can exhale, and how quickly. There are several types of pulmonary function graphs that show data from the tests. Some of the things that tests measure include:
- FVC (forced vital capacity) is the total amount of air you can exhale in a single, prolonged breath.
- FEV1 (forced expiratory volume in one second) is the amount of air you exhale in the first second. FEV1 is often expressed as a percentage of FVC.
- FEV1/FVC is the amount of air exhaled in the first second compared to the total amount of air exhaled. It’s given as a ratio (fraction) or a percentage. In general, the higher the FEV1/FVC, the better.
- PEF (peak expiratory flow) is a measure of how fast you can exhale. It can be tested with spirometry or a peak flow meter.
- RV (residual volume) is the amount of air left in the lung following a maximal exhalation.
- FRC (functional residual capacity) is the amount of air that remains in our lung, as we breathe normally at rest.
- TLC (total lung capacity) is the total amount of air that our lungs can hold after taking a maximal inhalation.
- DL (diffusion of the lung) is a measurement that reflects gas exchange (such as oxygen) in the lung.