Medical College of Wisconsin Geriatric Psychiatry Fellowship
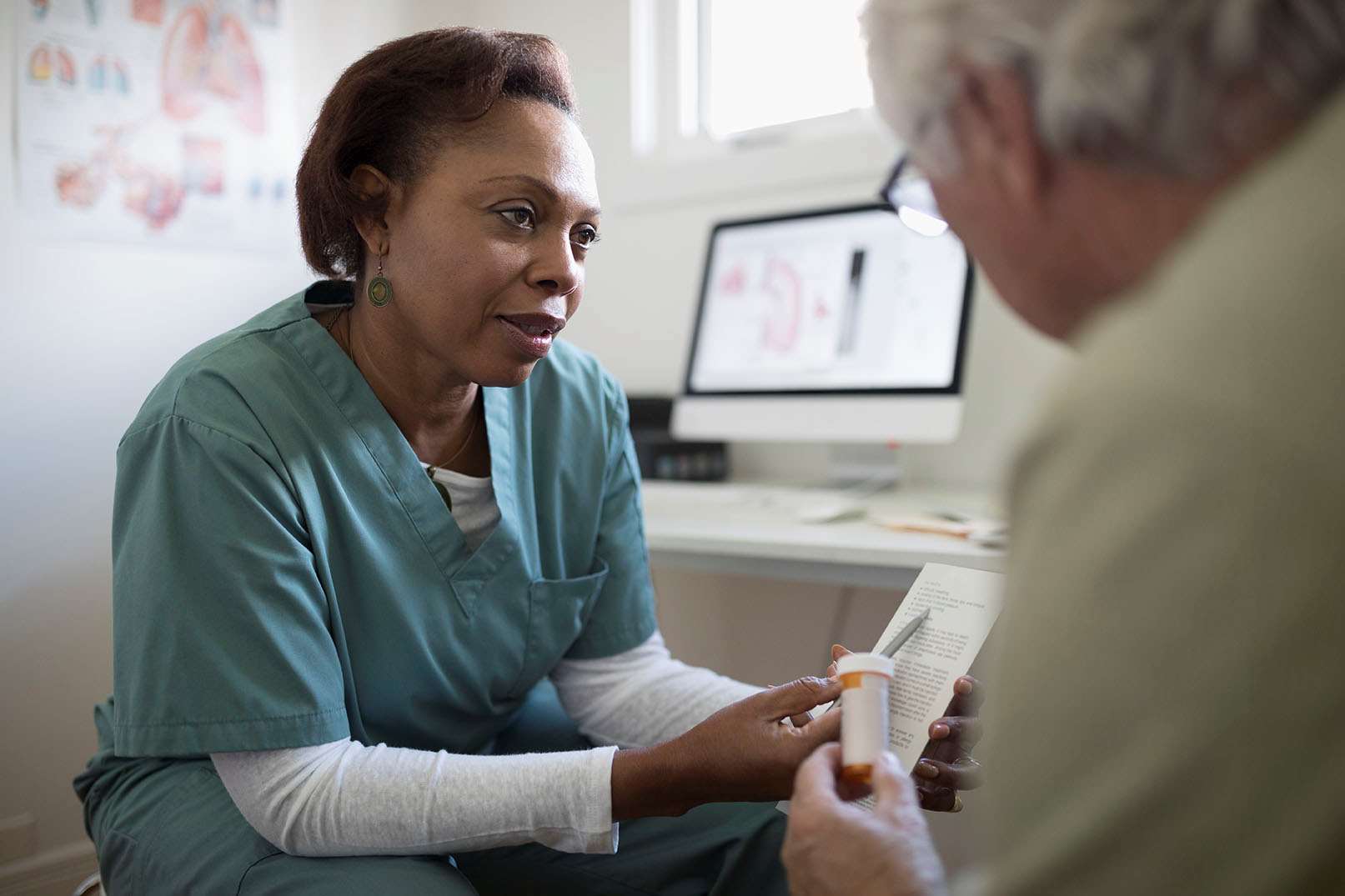
Geriatric psychiatry is an interesting and important field at the intersection of psychiatry and medicine. Individuals who become geriatric psychiatrists tend to be independent thinkers who enjoy older adults and welcome the challenges of staying up-to-date in medicine, neurology, psychopharmacology, and end-of-life issues. Care for the geriatric psychiatry patient requires appreciation for their family, care system, cultural framework, and the social structure in which they live. Access to knowledgeable and competent psychiatric care for older adults is a growing but underserved need.
The Medical College of Wisconsin’s ACGME-accredited geriatric psychiatry fellowship is designed to train the next generation of clinical and academic leaders in the field of geriatric psychiatry. Upon successful completion of the program, fellows will be eligible to take the American Board of Psychiatry and Neurology (ABPN) Examination for Added Qualification in Geriatric Psychiatry.
The program is closely linked with the ACGME-accredited MCW Geriatric Medicine Fellowship program and the MCW Department of Neurology. Fellows gain comprehensive knowledge in the adaptive and maladaptive responses to the biological and psychosocial changes associated with aging, psychopathology beginning in and continuing into late-life, psychiatric aspects of medical and neurocognitive disorders, evidence-based pharmacotherapy, psychosocial- and community-based interventions in treating late-life mental and neurocognitive disorders, and the social, cultural, legal and ethical issues pertinent to geriatric psychiatric disorders and their treatment.
Application Process
The Geriatric Fellowship Program at the Medical College of Wisconsin has two (2) positions and accepts ongoing applications. Interested applicants should complete the MCWAH application form and submit it to the Department of Psychiatry along with the necessary items from the application packet list. Typically, interviews take place in the fall for the upcoming academic year. Our program does not utilize ERAS.
Interested applicants must submit a completed application packet with the following items:
Application Packet
- MCWAH application form (PDF)
- Current curriculum vitae (gaps in time greater than one month must be explained)
- Personal Statement explaining your interests and goals
- Original Transcript of Steps 1, 2 and 3 Scores (must pass all 3 steps before applying)
- Medical School Dean’s Letter
- Medical School Transcript
- Copy of Medical School Diploma
- ECFMG Certificate (international medical school graduates)
- Visa Status Information (international citizens)
- 3 Letters of Recommendation
- One of the letters should be from your current training director and include your residency training summary.
- Letters of recommendation should be addressed to Dr. Katherine Levine and sent directly to the Medical College of Wisconsin.
Once all items have been obtained, email the complete application packet to:
Program Director: Dr. Katherine Levine at klevine@mcw.edu
c/o Fellowship Coordinator, Beverly Hayes at bhayes@mcw.edu
All accepted candidates are required to hold a valid Wisconsin Medical License and DEA certificate before starting the program. View information about Graduate Medical Education website. For questions please contact the Fellowship Coordinator.
Didactics and Supervision
The fellows participate in scheduled seminars on the topics of biology and cognitive changes in aging, psychopathology, and psychotherapeutic and psychopharmacological interventions for various geriatric psychiatric disorders. Additionally, psychiatric aspects of long-term care, as well as the social, cultural, ethical, legal and administrative issues relevant to practice of geriatric psychiatry are explored. Geriatric psychiatry case conferences and journal clubs are an important part of the fellowship didactics. Fellows participate in the Fellows Most Difficult Case Conference, and they also participate in the Geriatric Psychiatry Colloquium, a multi-institutional learning experience with fellow geriatric psychiatry fellows as well as geriatric medicine fellows. In addition to our core didactics, we provide a wide variety of optional educational didactics in such fields as palliative medicine, sleep, PM&R, and geriatric medicine. Participation in the American Association of Geriatric Psychiatry annual meeting is encouraged.
The geriatric psychiatry fellows supervise and teach medical students and general psychiatry residents during many of their rotations. All fellows perform scholarly activities in the form of lectures to residents, departmental grand rounds, and/or peer-reviewed publications. All fellows complete a QI project. A variety of electives are available, including eConsults, palliative care, addictions and research. In addition to the clinical supervision available from geriatric psychiatry fellowship program faculty, fellows receive individual supervision on a weekly basis.
Clinical Rotations
Clinical Rotation Sites
Elective Rotations
Meet The Team
Director | Katherine Levine, MD
Dr. Katherine Levine is an assistant professor at the Medical College of Wisconsin and associate residency program director for the Department of Psychiatry and Behavioral Medicine. Dr. Levine’s undergraduate education was at the University of Minnesota. She attended medical school at Albert Einstein College of Medicine in New York and her psychiatry residency and geriatric psychiatry fellowship were at the Perelman School of Medicine at the University of Pennsylvania.
Closely involved in resident, fellow, pharmacy school and medical student education; Katherine Levine has received the MCW Outstanding Medical Student Teacher award from 2015-2018 and 2021-2022. Her involvement in professional organizations includes the American Association of Geriatric Psychiatry as well as the American Association of Directors of Psychiatric Residency Training. She has contributed to recent textbooks including the Companion to the American Psychiatric Publishing Textbook of Geriatric Psychiatry, Emergency Psychiatry: Principles and Practice, Geriatrics Review Syllabus 11th edition, and Essential Reviews in Geriatric Psychiatry. Dr. Levine is a invited presenter at the Bi-Annual Wisconsin Update in Geriatric Medicine and is a Geriatric Fast Facts contributor.
Coordinator

Faculty

Travis Fisher, MD
Associate Professor

Joseph S. Goveas, MD
Professor, Psychiatry and Behavioral Medicine and Institute for Health & Humanity; Vice-Chair and Director, Geriatric Psychiatry

Harold H. Harsch, MD
Professor

Thomas W. Heinrich, MD
Professor; Vice Chair

Cary J. Kohlenberg, MD, DLFAPA
Assistant Clinical Professor

Makenzie Hatfield Kresch, MD
Adjunct Assistant Professor; Associate Program Director, Geriatric Psychiatry Fellowship Program

Eric R. Larson, PhD, ABPP-CN
Associate Professor

Katherine Levine, MD
Assistant Professor

Deepa Pawar, MD, MPH
Assistant Professor
Recent Fellows
Makenzie Hatfield Kresch, MD
Adjunct Assistant Professor; Associate Program Director, Geriatric Psychiatry Fellowship Program

Hannah Reiland, DO
Fellow
Medical School: Des Moines University College of Osteopathic Medicine; Residency: Medical College of Wisconsin
Contact Us
The Geriatric Fellowship is accredited by the American Council for Graduate Medical Education (ACGME).
Beverly Hayes
Program Coordinator