Language Therapy Program Offers Hope to Aphasia Sufferers

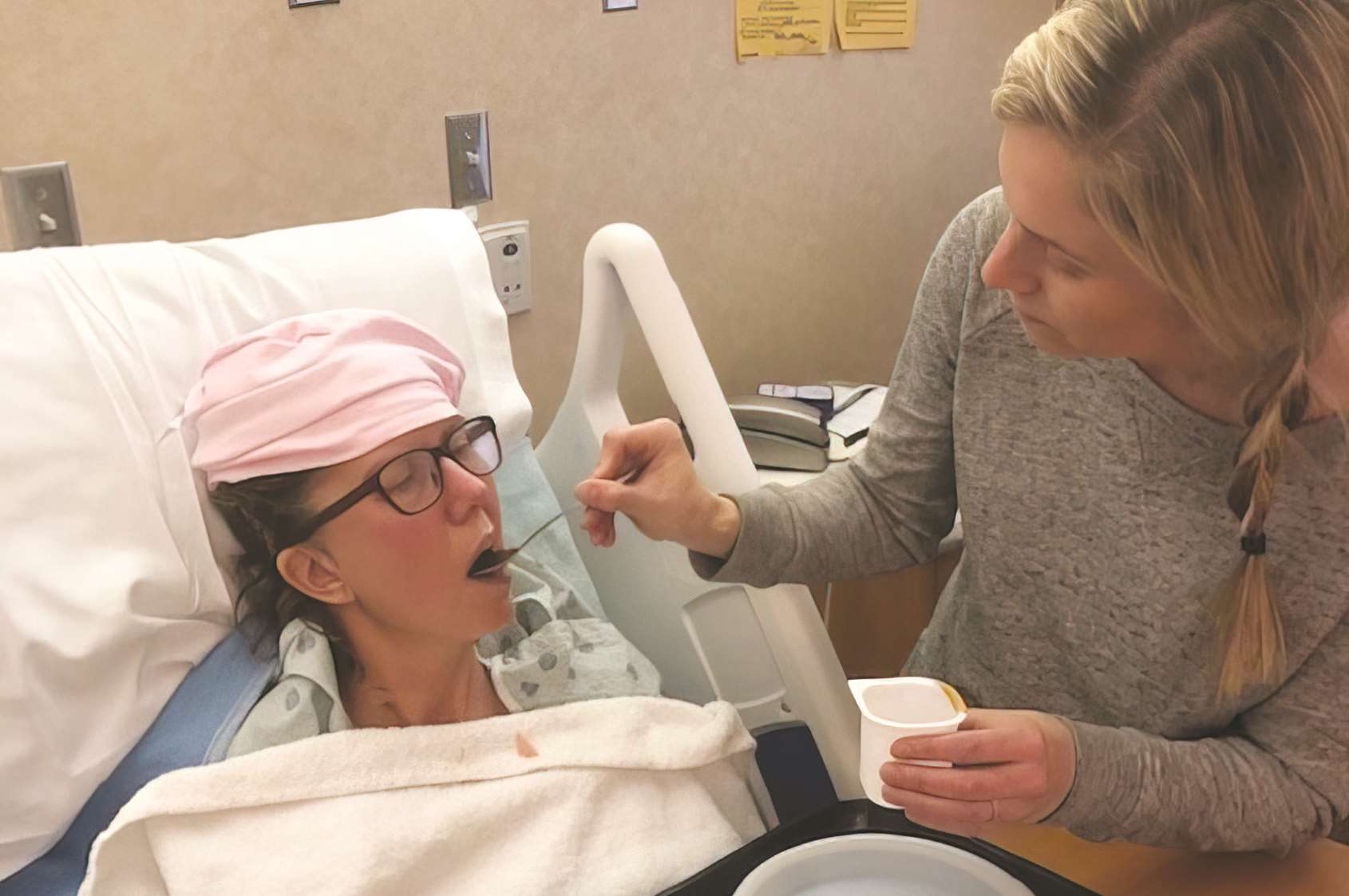
Lori Johnson, who is recovering from a massive stroke that resulted in aphasia, credits MCW’s IPAT comprehensive language therapy program with helping her to regain some of her ability to speak.
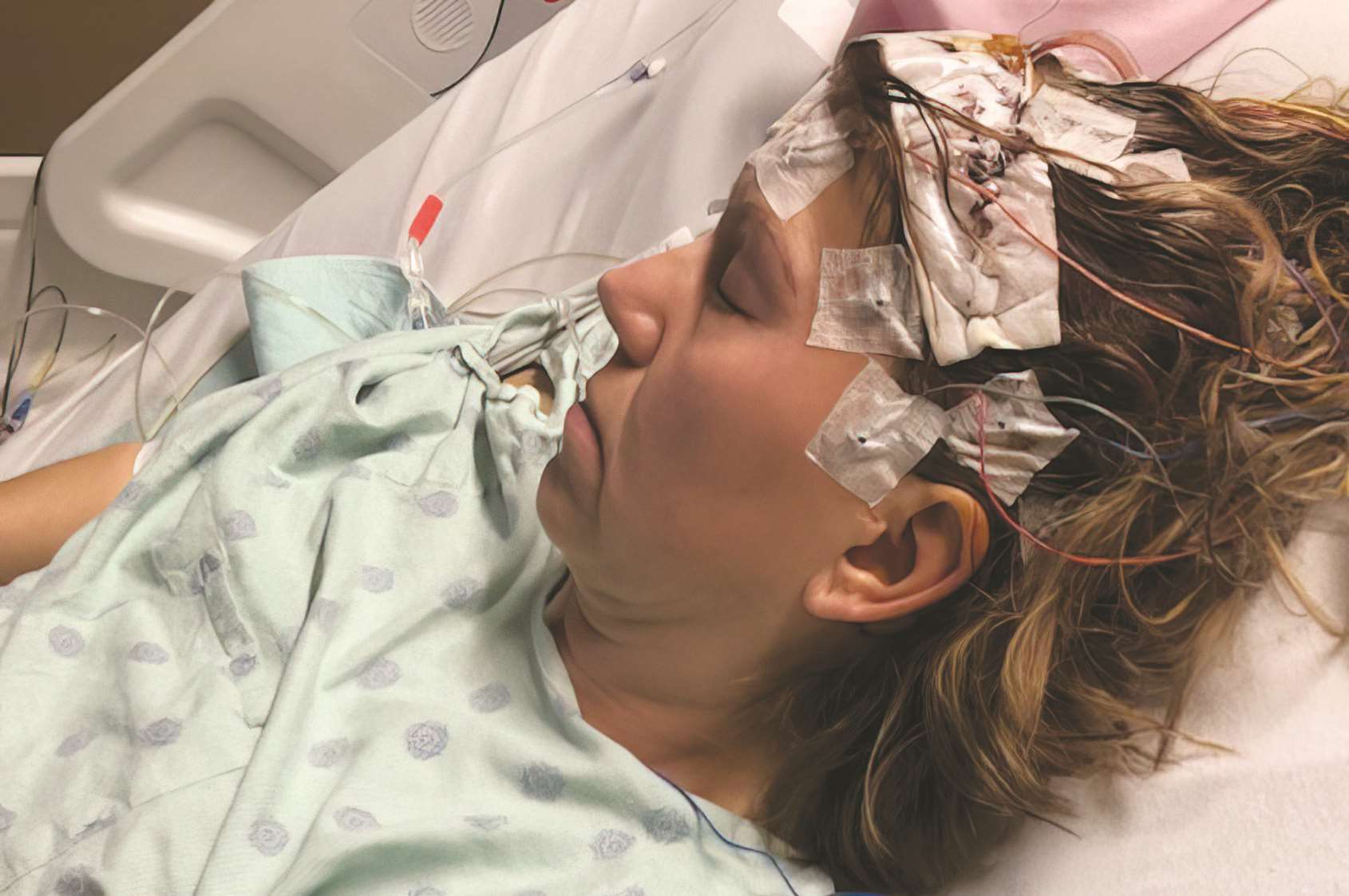
Lori Johnson and her family know the struggles of aphasia all too well. At age 55, this healthy mother and grandmother suffered a massive left hemorrhagic stroke. Although Johnson survived, it limited her ability to use the right side of her body and resulted in aphasia, a debilitating disease which affects roughly 180,000 individuals each year.
Aphasia impacts one’s ability to speak, write or understand spoken and written language, according to Sara Pillay, PhD, GME ’16, FEL ’18, MCW assistant professor of neurology. In addition to relearning to walk, aphasia would force Johnson to learn to communicate independently again. “Aphasia is very socially isolating,” says Dr. Pillay, adding that it also regularly causes long-term disability because patients are not able to return to work. “Patients may experience frustration, shame or embarrassment from not being able to communicate.”
This stigma, and advocating for the condition, makes aphasia less well known than other diseases such as Parkinson’s and multiple sclerosis, even though it’s more common, Dr. Pillay shares. According to the National Institute on Deafness and Other Communication Disorders, in the US, approximately one-third of all strokes result in aphasia, and one out of every 272 Americans are affected with this condition.
Care for aphasia typically involves treating the symptom that caused it together with speech and language therapy. Unfortunately, according to Dr. Pillay, insurance often limits the amount of therapy a patient can receive to treat aphasia. “If a patient reaches their visit limit for a year, or if progress starts to plateau, insurance will no longer pay for speech therapy – leaving these patients without additional options and limiting their ability to recover,” she says.
Experts told Johnson that her language would not progress further after initially beginning rehabilitation. The news crushed her family. “It scared us, too,” says her daughter, Nicole McGonigle. “However, we knew my mom would never give up.” She was right. Johnson simply told them, “No way.”
Program Offers Hope
As part of her recovery, Johnson was invited to participate in the Intensive Program of Aphasia Therapy, or IPAT, a comprehensive language therapy program at MCW, directed by Dr. Pillay and Jeffrey Binder, MD, MCW professor and vice chair of research in the department of neurology and director of MCW’s Language Imaging Laboratory.
Led by a multidisciplinary team of experts in speech therapy, neurology, neuropsychology and biomedical engineering, IPAT helps people such as Johnson regain their ability to communicate through intensive, cutting-edge and evidence-based treatments tailored to the patient’s individual needs.
“The IPAT Clinic was developed to provide an intensive speech therapy program for individuals who have maxed out of traditional speech therapy options covered by insurance, but yet would still benefit from additional intervention,” Dr. Pillay says.
The program begins with an assessment that involves compiling a detailed profile of the strengths and weaknesses of each participant. Using that knowledge, along with information gleaned from more than 20 years of research conducted at MCW regarding the location of language processes in the brain, the speech therapy team crafts a unique plan that targets these weaknesses and works on compensatory measures, Dr. Pillay shares. The two-week therapy program runs four hours a day on weekdays; in total, patients receive 40 hours of individual and group therapy. Research on aphasia treatment has found that many hours of therapy over a shorter timeframe may have more impact than standard speech therapy.
Another important aspect of the program is the support patients receive from other participants. “Most of these patients have never heard another patient with aphasia talk,” says Dr. Pillay. “So, this is a big communication and morale booster.”
IPAT is sponsored in part by a generous donation from the We Energies Foundation.
Contributing to Clinical Research
McGonigle says being able to communicate with others with aphasia was a big help for her mother. “She loved the social aspect of it and felt very comfortable with everyone,” McGonigle shares.
An additional component of the program – one which could lead to major advances in aphasia care – is the opportunity for participants to be part of clinical research studies that involve brain stimulation techniques.
Helping to lead this aspect of IPAT is Priyanka Shah-Basak, PhD, MCW assistant professor of neurology. Dr. Shah-Basak has a background in biomedical engineering and became interested in neuro rehabilitation as a postdoctoral researcher. Her initial work was focused on improving and optimizing brain stimulation to enhance rehabilitation efforts, which led her to research on language impairment and aphasia. The research component of IPAT furthers her work. “IPAT enables us to learn more about these treatments and also how brain stimulation increases efficacy,” she says.
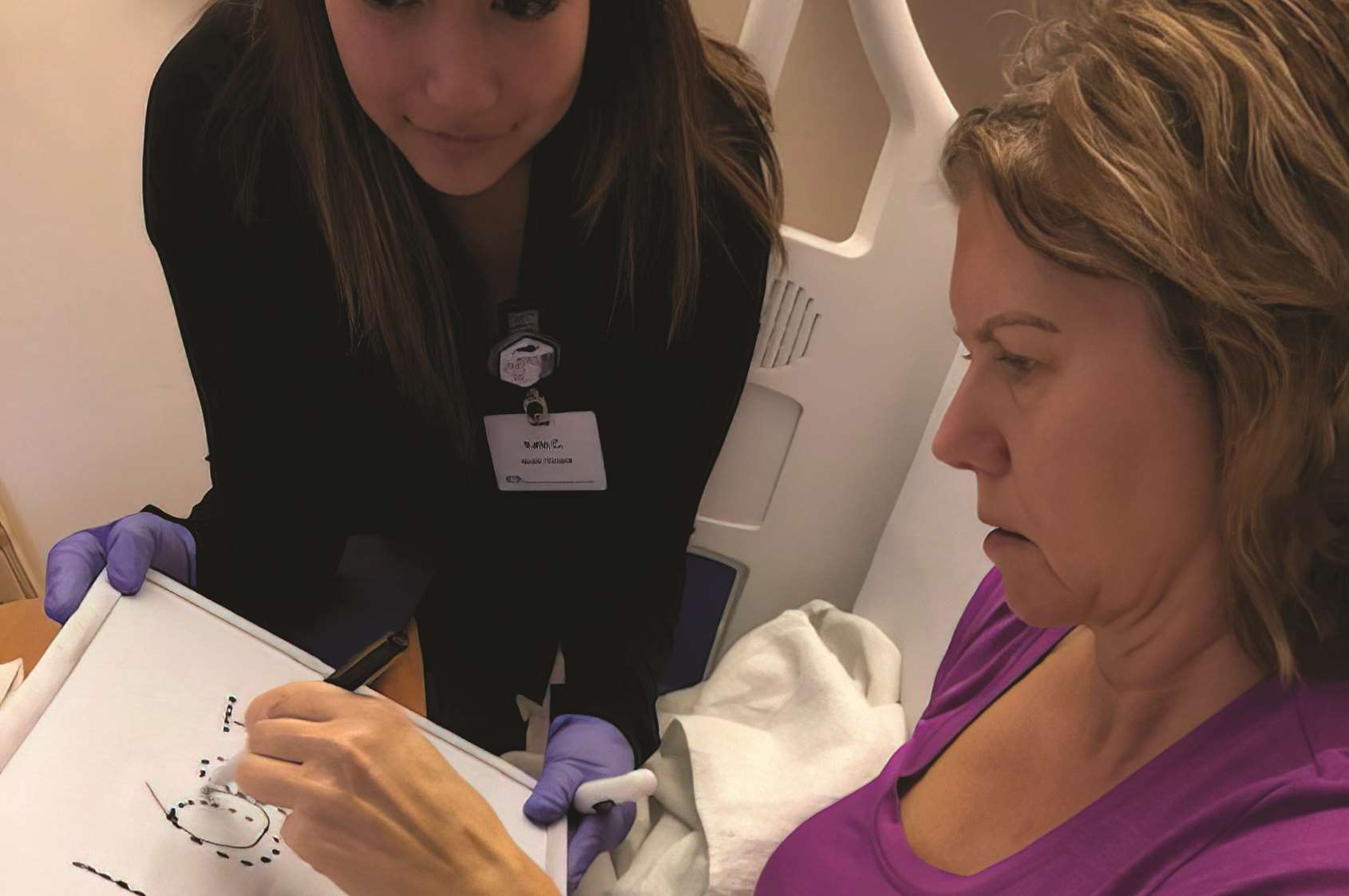
The brain stimulation used in the research project occurs externally, as electrical leads are placed on the scalp to target precise locations of the brain, Dr. Shah-Basak shares. Targeting brain regions involved during therapy using positive (or “anodal”) stimulation leads to excitation or increases in activation of those areas and helps researchers learn how to enhance future treatments. “This research uses prior neuroimaging work at the group level to probe specific linguistic processes that we’re targeting with therapy among individual patients,” she says.
For those who are wary of electrical stimulation, Dr. Shah-Basak notes that the sensations are mild and considered to be very safe. “There could be mild effects – tingling, a little bit of itchiness afterwards and some redness from stimulation that is done over time,” she adds.
While studying specific brain stimulation techniques remains a challenge because each individual’s brain reacts differently to treatment, new technologies such as high-definition stimulation have helped researchers better target treatments to a smaller section of the brain.
The ultimate goal of the research and treatment is to help patients regain what they have lost: the ability to functionally communicate. “This loss can have an impact on the social communication abilities with their family members, or on the ability to return to work or do better at work,” according to Dr. Shah-Basak. Johnson – who also participated in the brain study – says that the program has helped her regain some of her ability to speak. Along with taking regular walks again, she is able to order food at a restaurant once more. “It feels so good to be able to do these things again,” Johnson says.
– MCW Magazine Staff
Lori Johnson is pictured in the hospital immediately after suffering a massive left hemorrhagic stroke, during her recuperation and participating in MCW’s IPAT program to help her regain the ability to functionally communicate.