Medical College of Wisconsin Combined Internal Medicine/Psychiatry Program

We are looking for innovators, integrators, and ignitors of change.
So much is happening at MCW in the Behavioral Health integration movement – it’s the perfect time for dual-board training here.
Funded by both the Milwaukee VA and Froedtert Health, the combined program capitalizes on the strengths of both categorical programs while building its own identity with Med/Psych rotations and didactics. We have a wealth of dual-boarded faculty working in Consult-Liaison, Perioperative Medicine, Integrated Behavioral Health in Primary Care, and Psych-Oncology.
Med/Psych residents at MCW are pioneering new programs and improving existing integrated efforts at the VA while leading our new Complexity Intervention Unit at Froedtert Hospital to care for acutely comorbid patients.
Program Highlights
- Our combined residents will have significant leadership opportunities in program development and will be asked to provide interdisciplinary education.
- There are ample opportunities for scholarly activity within both sponsoring departments.
- Competitive applicants will be able to articulate how combined training will help their future patients and the health care system.
Reasons to live in Milwaukee
Program Requirements
Internal Medicine
- 30 months total of internal medicine
- 4 weeks of emergency room during years 1 or 2
- 4 weeks of care for ICU during years 1 or 2
- 4 weeks of care of ICU during years 3, 4, or 5
- At least 33% (thus 10 months of 30 Medicine months) must involve ambulatory experiences
- Continuity clinic
- At least 4 months of subspecialty experiences (inpatient, outpatient, or a combination)
- Significant exposure to inpatient cardiology
Psychiatry
- 30 months of psychiatry training
- 2 months of neurology (1 month in either PGY1-2, and 1 month in PGY3-5)
- Between 6 and 16 months of inpatient psychiatry
- Inpatient geriatric, addiction, and/or forensics can count as inpatient psych months but only above an initial 6 months of general inpatient psychiatry
- 12 months of organized, continuous, and supervised clinical experience in outpatient treatment with experience in both brief and long-term care of patients
- 2 months of child and adolescent
- 2 months of consultation-liaison psychiatry
- 1 month of geriatric psychiatry (inpatient or outpatient)
- 1 month of addiction psychiatry
- Exposure to the evaluation of forensic issues including writing a forensic report
- Exposure to an organized 24-hour psychiatry emergency service, a portion of which may occur in ambulatory urgent-care settings
- Exposure to community psychiatry (community-based settings, crisis teams, public hospitals, community mental health centers)
Sample Rotation Block Grid
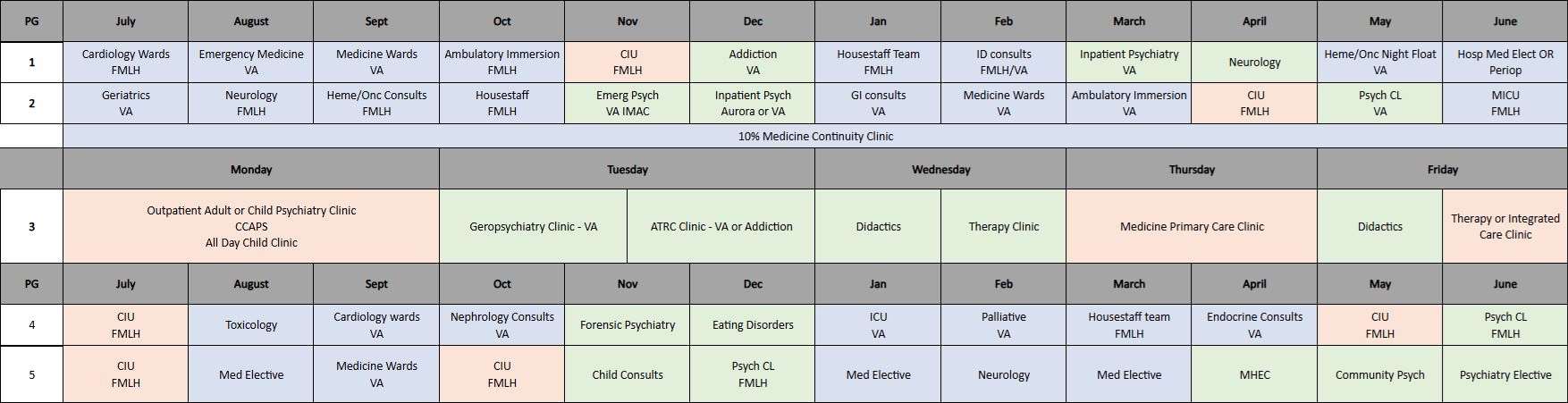
Key:

- Residents will have training at a wide variety of sites including VA, Froedtert Hospital including the CIU, Aurora, Rogers, MHEC, Tosa Health Center, Children’s Wisconsin.
Frequently Asked Questions
Meet Our Team

Amalia J. Lyons, MD
Associate Professor

Sara Lindeke, MD
Associate Program Director, PGY1, Milwaukee Psychiatry Residency Program; Associated Program Director, Internal Medicine Psychiatry Combined Residency Program; Assistant Professor, Department of Psychiatry and Behavioral Medicine

Corinne Palmer
Internal Medicine Psychiatry Combined Residency Program Coordinator

Sara Brady, MD
Program Director Categorical Psychiatry Residency; Assistant Professor

Kathlyn Fletcher, MD, MA
Program Director Categorial Internal Medicine; Co-Director, Graduate Medical Education Pillar; Professor of Medicine; Member, Clinical Learning Environment Pillar, Kern Institute
Other Dual Boarded Faculty

Lisa Wehr Maves, MD
Assistant Professor

Thomas W. Heinrich, MD
Professor; Vice Chair

Jennifer Knight, MD, MS, FACLP
Professor, Psychiatry and Behavioral Medicine and Microbiology & Immunology
Contact Us
Follow us on social media

