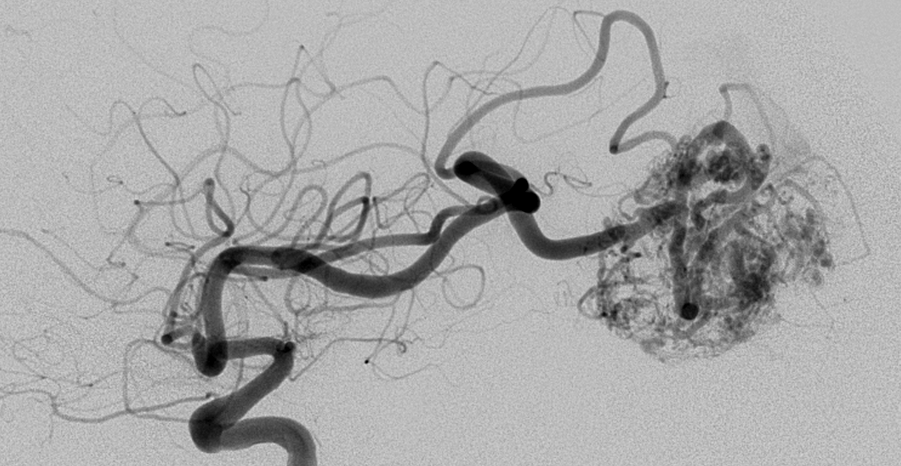
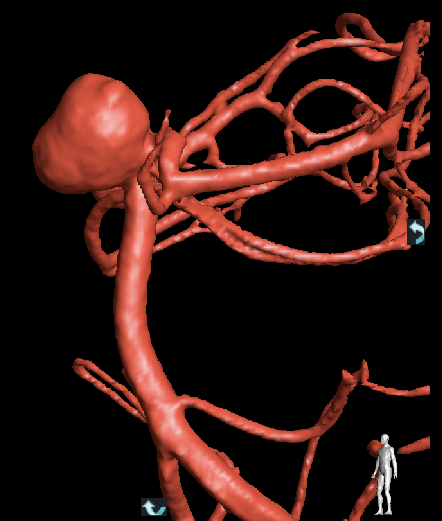
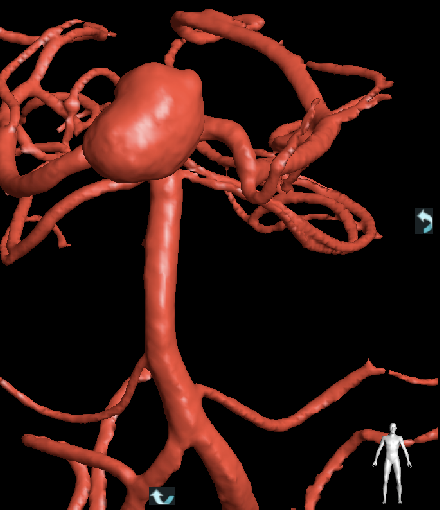
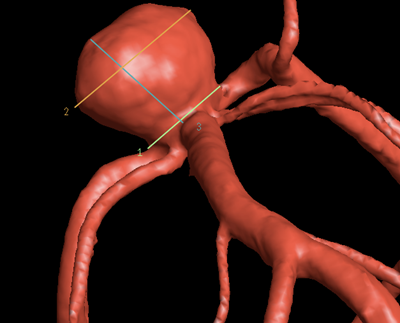
Medical College of Wisconsin Stroke, Neurointervention, and Critical Care
Meet Our Stroke Neurointervention & Critical Care Team

Hatim Attar, MD
Interim Division Chief, Neurology at Zablocki VA Medical Center; Assistant Professor
Specialty: Inpatient Stroke



Marek Cierny, MD
Assistant Professor
Specialty: Inpatient Stroke


Joshua E. Medow, MD, MSc, PhD, FAANS, FACS, FNCS, FAHA, FCCM, FAMIA
Division Chief, Inpatient Neurology; Professor
Specialty: Adult Neuro ICU


Adam C. Wadina, MD
Assistant Professor
Specialty: Vascular Neurology/Stroke (Ambulatory & Inpatient)
Department Info
Selected Disorders and Conditions
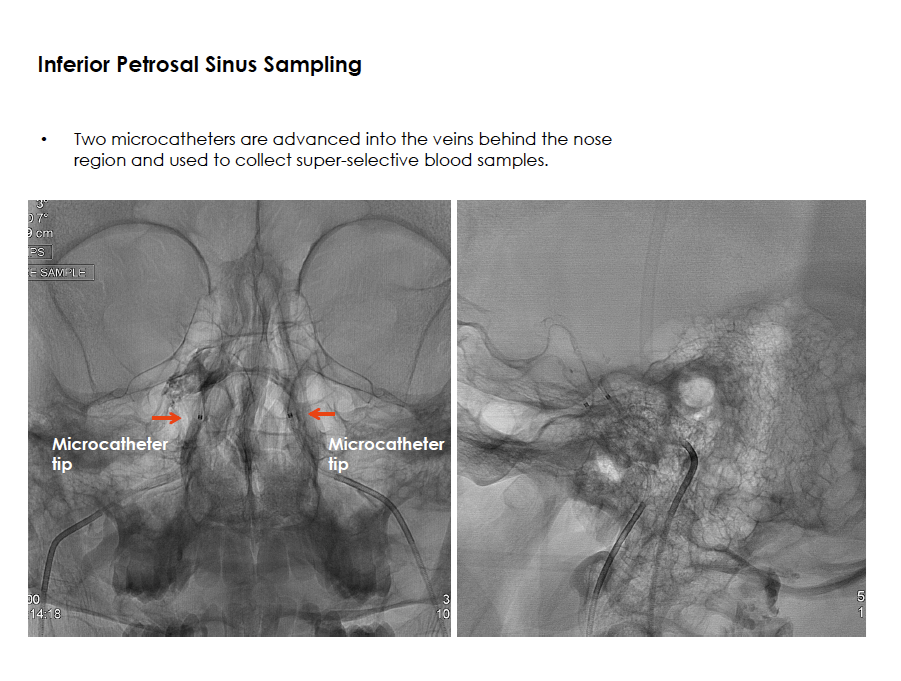
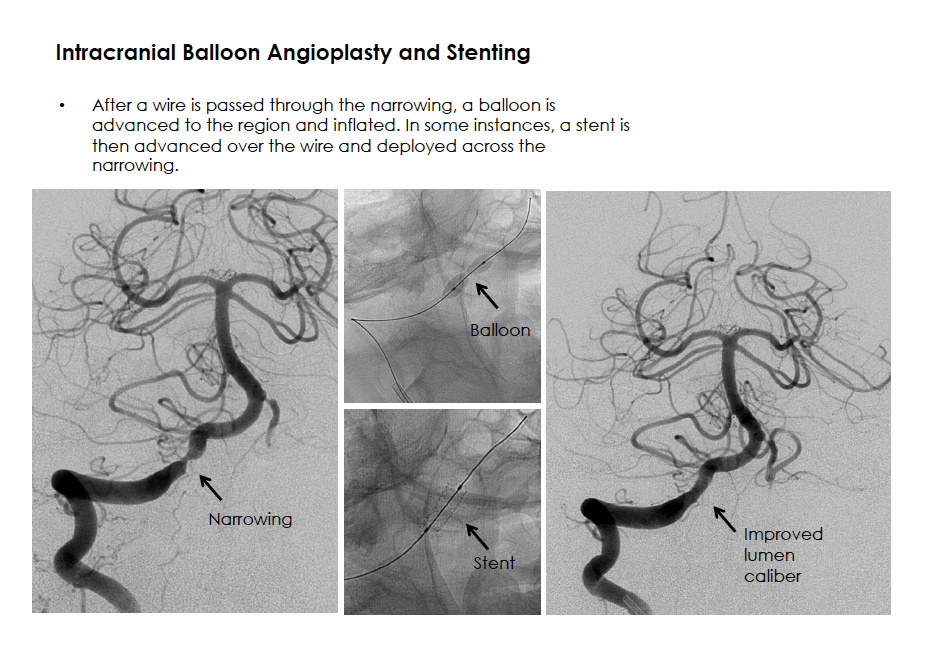
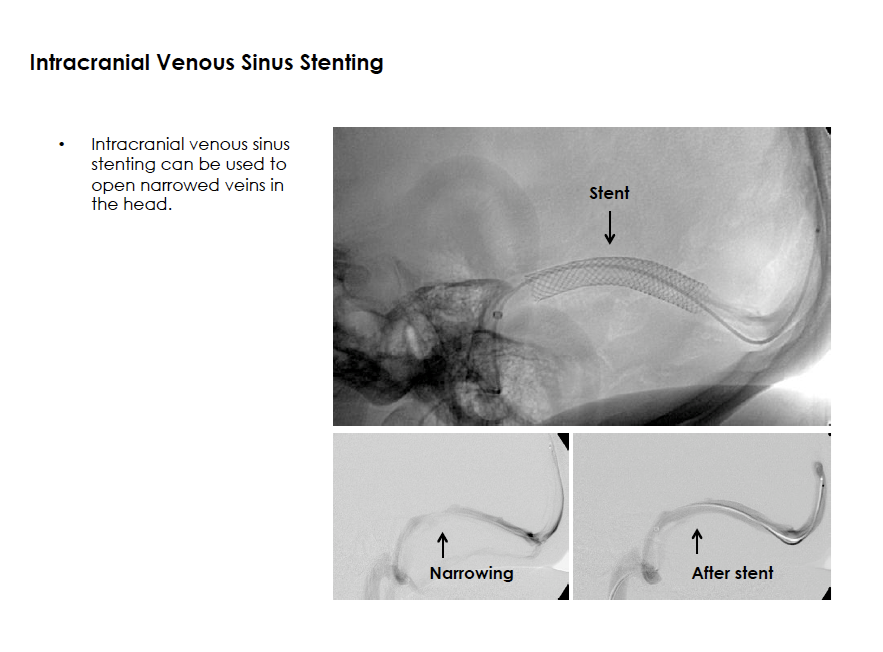
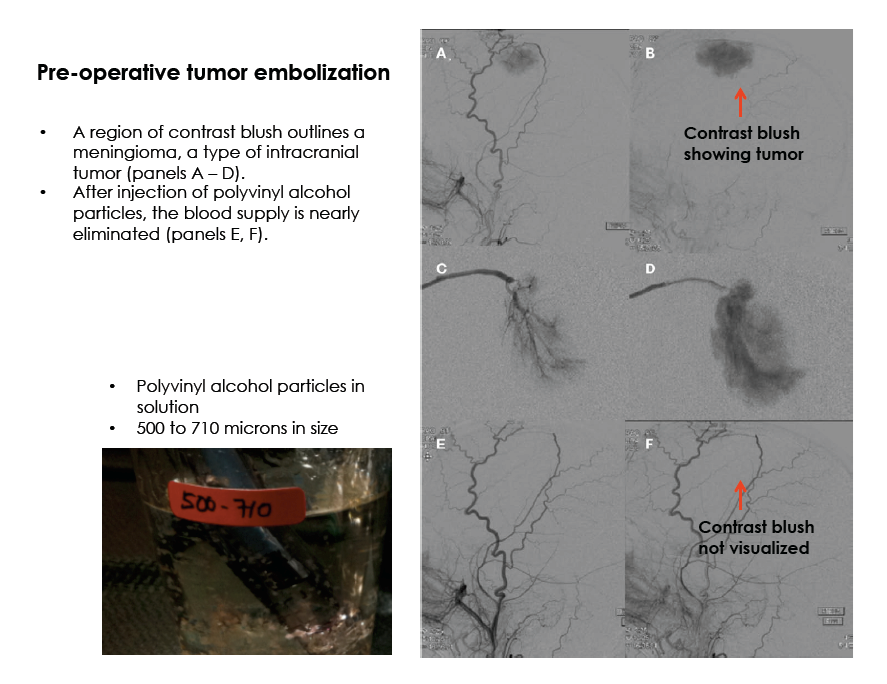
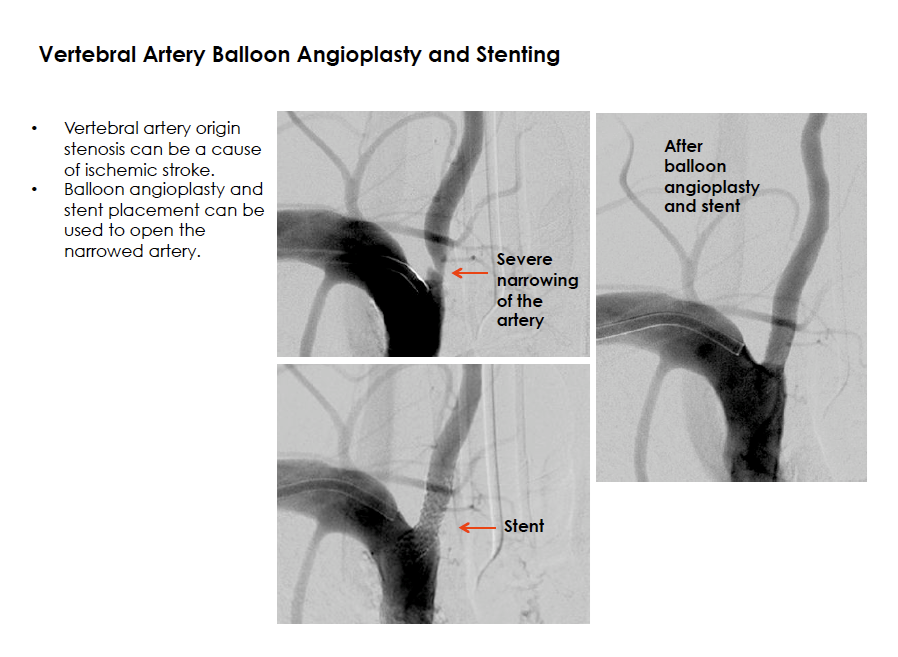
Selected Procedures
Disclaimer
The information on the Division of Stroke, Neurointervention and Critical Care website is for educational purposes only and is not intended as medical advice. While general information regarding the conditions treated and procedures performed is posted, this information is not a substitute for professional medical advice, diagnosis, or treatment. All patients are treated with individualized care based on independent professional judgment and experience in each specific case.